DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
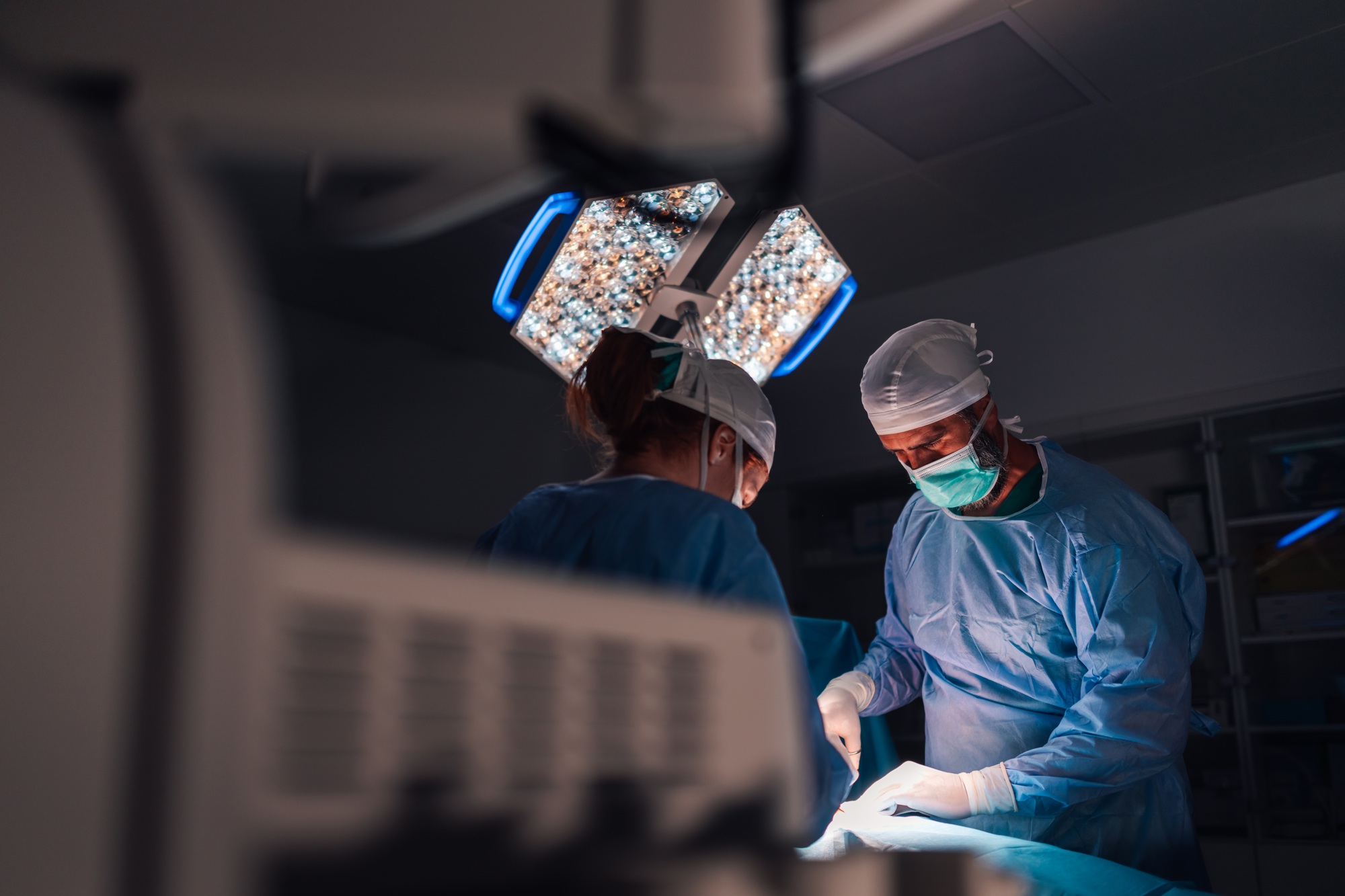
Knowledge is power, especially in the medical field. This remark is even more accurate when it involves the intensive care unit, which is “intense.” ICU staff often must make critical care decisions in minutes or seconds. The uncertainty of these decisions and the tension this engenders, coupled with stresses of ICU bed and staff shortages in the face of increased demand, especially during the recent COVID-19 pandemic, highlight the importance of access to data for decision support.
Big Data Knowledge Systems
As health care has become increasingly complex, the industry has recognized the need for a knowledge system that can support critical healthcare decision-making.
What is needed is the use of experience-based data gathered regarding patients’ diseases and treatments in order to determine the diagnosis, prognosis, and best treatment for future patients. Such clinical data could also offer new perspectives on complex problems. The challenge is how to transform and to integrate all this information into a functional, accessible, and practical medical knowledge system. An article published by online medical journal Critical Care in 2015 provided a then-advanced review of “the data revolution in critical care,” highlighting this need for better data systems to support decision-making. The authors articulate that “while the wetware of the human mind is a wonderful instrument,” the type of data integration that is needed exceeds standard cognitive capabilities.
eICU Database Introduced
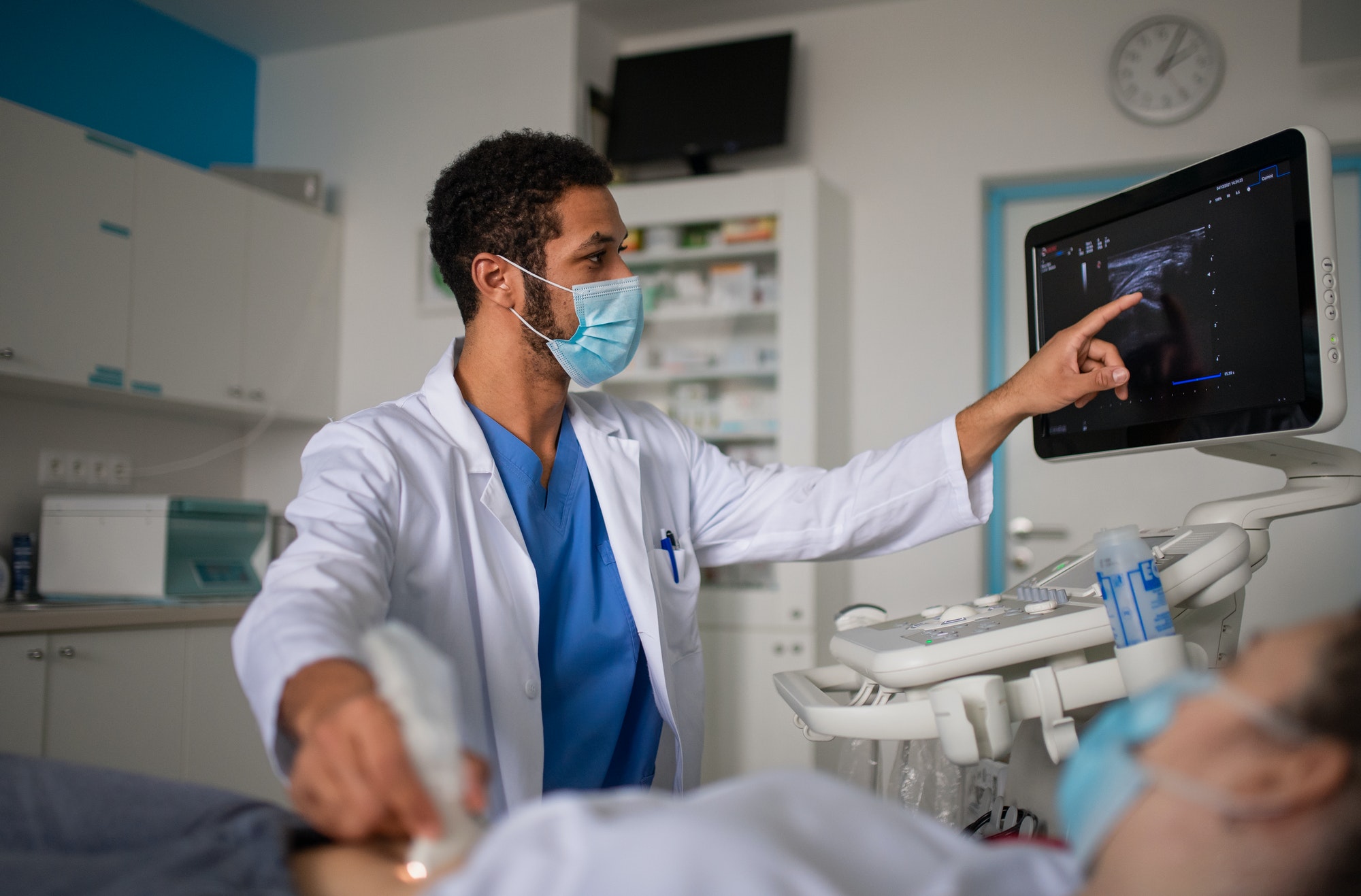
Since the COVID pandemic, there has been much buzz about the successes of eICU, Tele-ICU, remote ICU, virtual ICU, and virtual health – all of which refer to a centralized remote healthcare team working in support of intensive care units. A team may include board-certified physician intensivists, critical care nurses, and others, who are able to communicate with patients, their families and their intensive care unit bedside providers. The link is via state-of-the-art computer systems, enabling video visits using advanced audiovisual communication technology. The system enables the off-site eICU team to support and monitor critically ill patients simultaneously in ICUs in multiple units which may be in different hospitals that are geographically distant from each other.
The pandemic also brought the importance of information sharing to the fore. Access to patient EMRs is an essential component which enables the provision of eICU services. However, there have been hospitals and healthcare organizations who have resisted sharing this information. The integration of an HL7 standard interface into the TeleICU software has overcome many of these barriers and have improved access to information.
ICU physicians have long embraced the value of collecting and storing clinical records electronically. Their readiness to share information has led to partnerships between intensivists and academic or industrial entities. For instance, the commercial APACHE Outcomes database has laboratory and physiological measurements of over 1 million patient clinical records from 105 ICUs since 2010.
Another commercial database is the eICU Collaborative Research Database. The first version (v1.0) was released in December 2016 but was preliminary and not publicized widely, in order to allow for internal testing. The first public release was in March 2017, and the current version, eICU Collaborative Research Database v2.0., was released in May 2018.
What is the eICU Database?
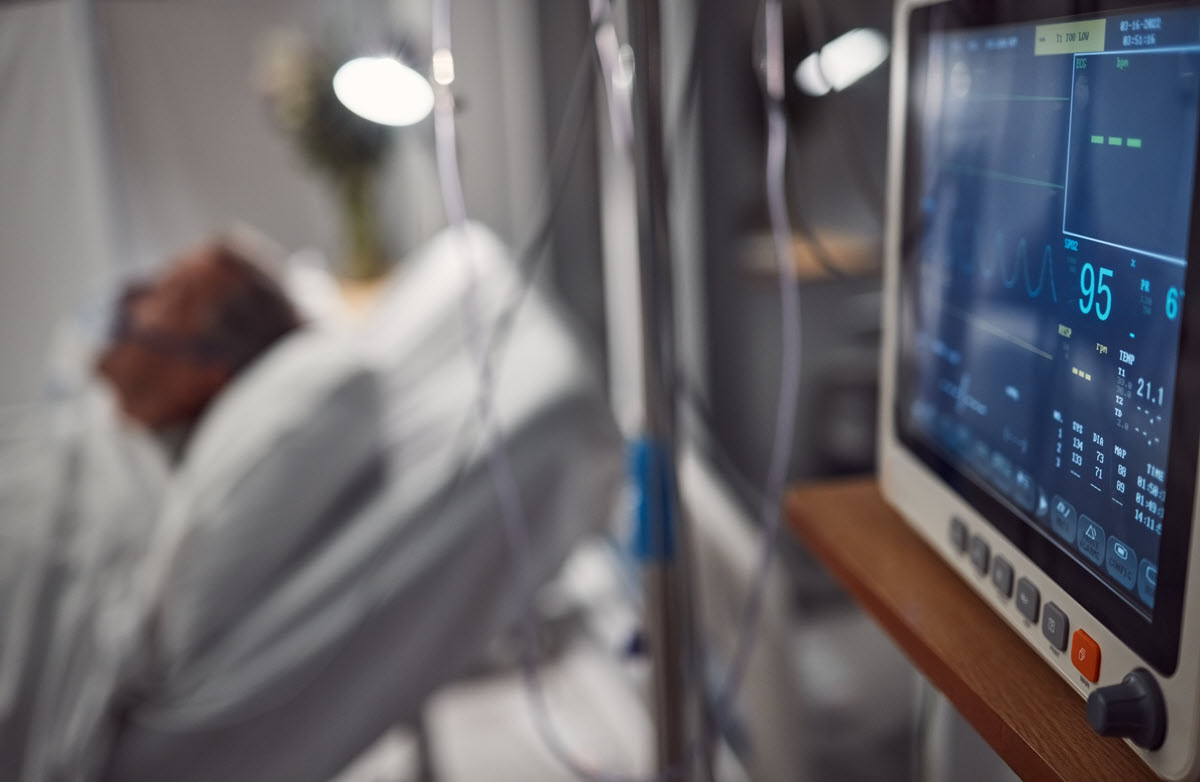
The eICU Collaborative Research Database is an extensive multi-center intensive care unit database that contains data for more than 200,000 patient admissions to eICU-monitored ICUs from 208 US hospitals between 2014 and 2015. The Database aims to provide a large sample size for research studies. The data are deidentified and contain patient care plans, vital sign measurements, APACHE severity of illness measures, diagnoses, treatments, and other information.
The Database website and documents are hosted publicly on GitHub (https://github.com/mit-lcp/eicu-code). By sharing the content, its creators hope to promote cooperation in the secondary analysis of EMRs. In their words, “we hope to foster a community around the eICU Collaborative Research Database, improving the efficiency of research by crowdsourcing knowledge generation.” Researchers are encouraged to send contributions, suggest improvements, and share code.
Key Takeaway
The care of critically-ill patients can be significantly improved by knowledge gained from the analysis of population-level databases which can enable physicians to make better-informed clinical decisions. Thus, data collected from many patients can be used to improve the medical care of the entire population.