DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
(*Note that the term “eICU” used here is used generically – to refer to Tele-ICU, telehealth ICU, virtual ICU — and does not refer to any brand of Tele-ICU in particular.)
Medical technology has come a long way since the stethoscope, the MRI, and the disposable catheter. Today, many factors including Covid-19, have forced healthcare into the 21st century, including a growing geriatric population, the rise in non-communicable diseases, and pervasive shortages of health workers. More than ever, AV (Audio Visual) and IoT (the Internet of Things) technologies have the most growth potential for the medical industry. Tech-inspired health systems and hospitals can also lead to substantial cost- savings into the millions if applied on a massive scale. Let’s look at the primary AV and eICU technology trends.
Retraining
According to the World Economic Forum, to keep pace with e-learning and e-health techniques, VR simulation, AI, and IoT, well over a billion healthcare workers need to retrain in medical technology by 2030. The industry must move into the Fourth Industrial Revolution. This move involves rapid scaling-up of emerging technologies, big data, and analytics, which will not only save more lives and reduce LOS but generate increased demand for new skills and employment opportunities in digital healthcare delivery.
Benefits of eICU
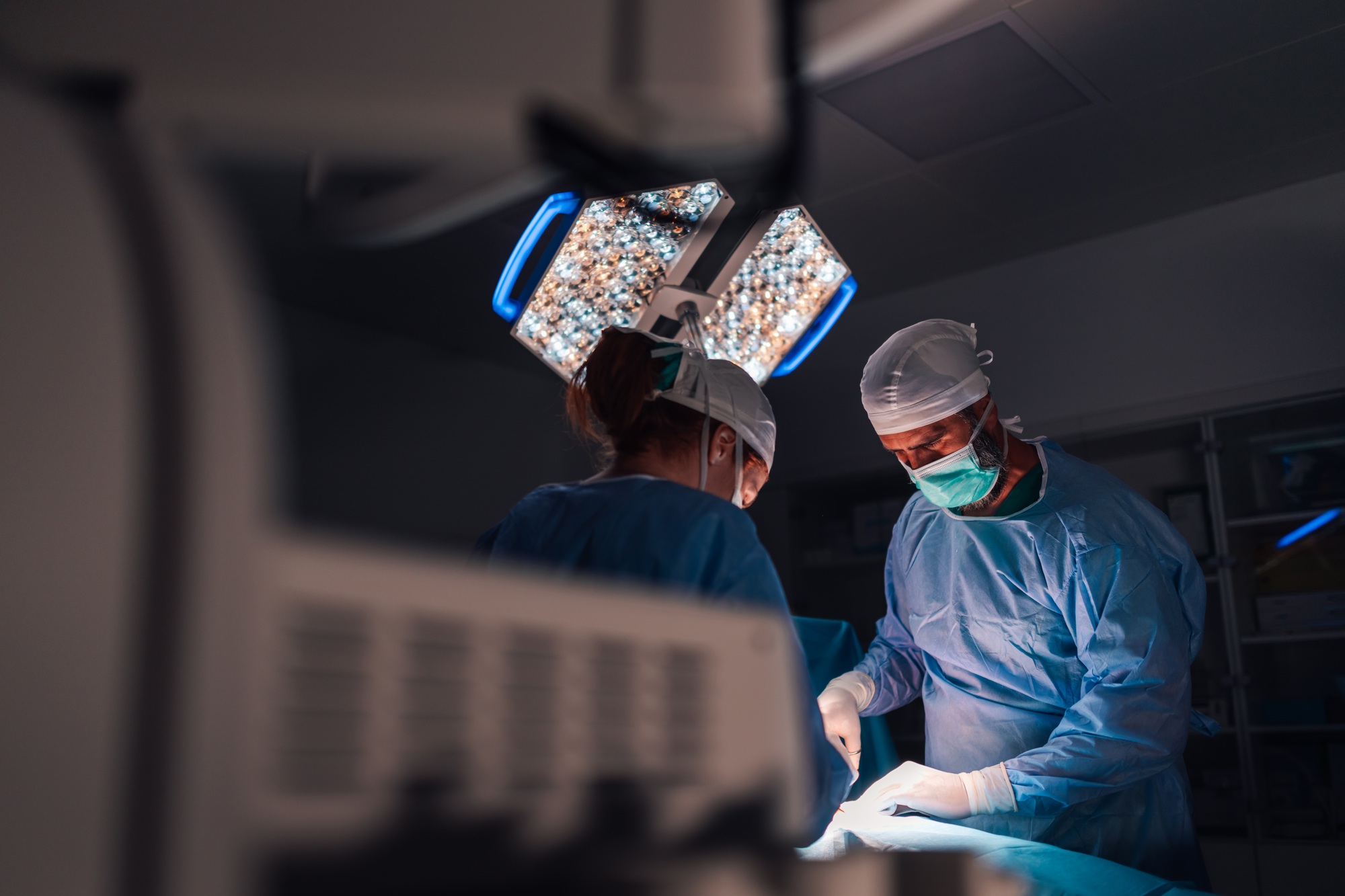
An Electronic Intensive Care Unit (eICU) is a critical care telehealth model that combines predictive analytics, A/V technology, data visualization, and advanced reporting capacities. Hospitals implementing these state-of-the-art platforms and devices have an added layer of critical care service to patients through real-time communication with remote central monitoring support centers staffed with intensivists, ICU medical care specialists, or ICU nurses with hospital ICUs. This automated 24/7 quality care access optimizes patient management and outcomes. It also dramatically enhances the abilities of lower-capacity or outlying hospitals and health systems.
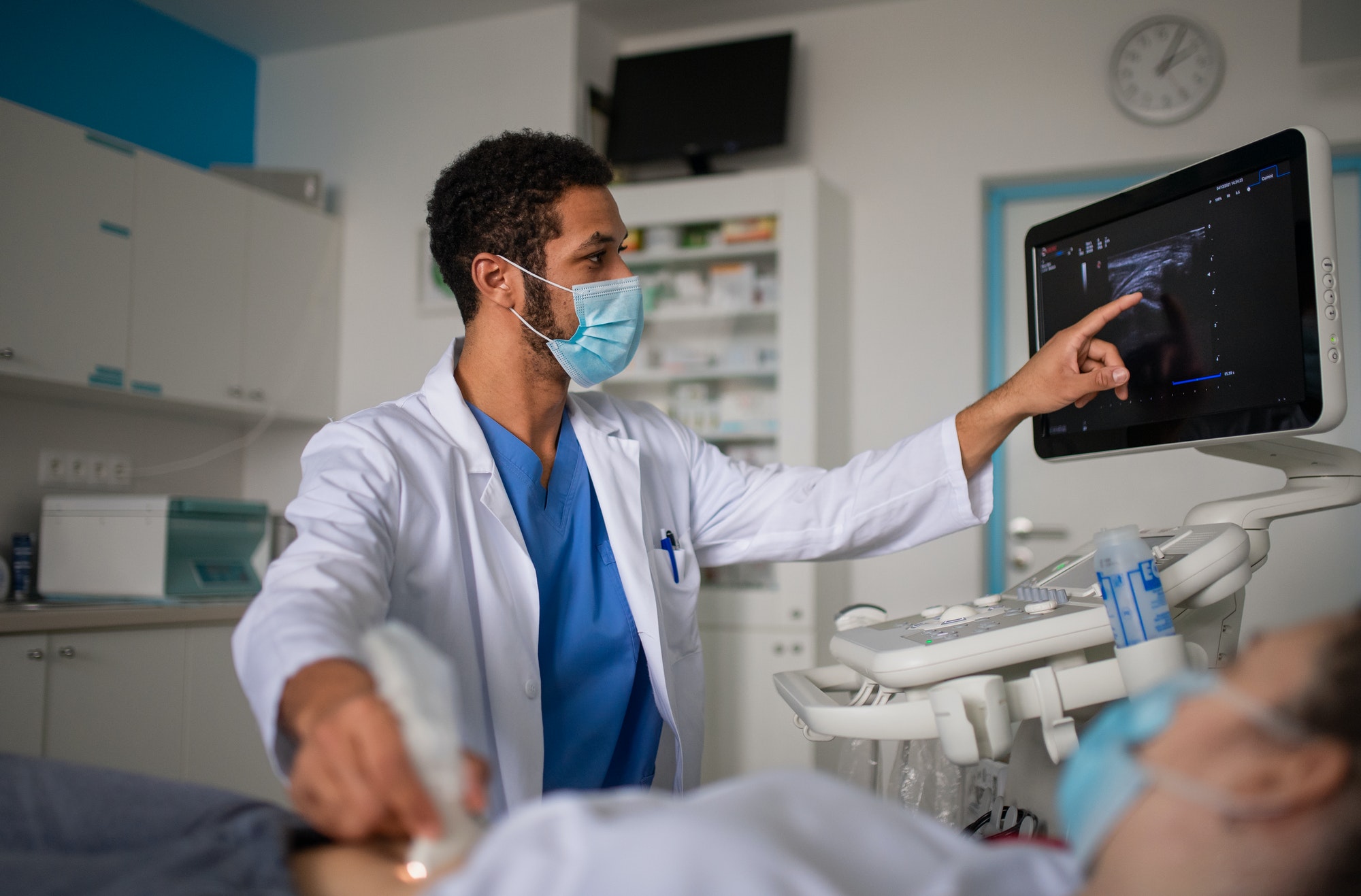
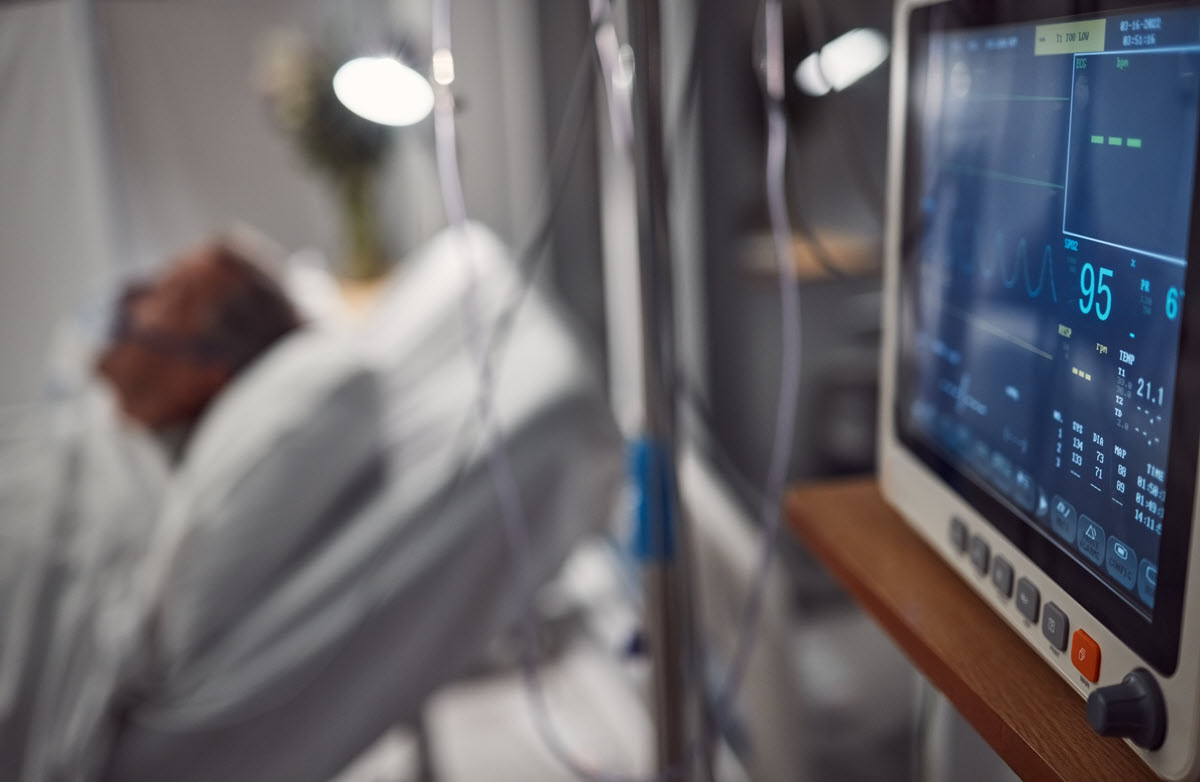
From the remote caregiver’s side, the platform allows access to clinical profiles, patient data, treatment information, and virtually entering a patient’s hospital room to check on their well-being and more. In an eIC setting, patients’ vital signs and conditions are monitored virtually via advanced AV equipment and software tools.
Furthermore, the off-site team can alert clinical providers and evaluate patient response to ongoing treatment. The onsite (bedside) clinical team can request a consultation with tele-intensivists, particularly in the case of an emergency (such as a code) or with difficult care decisions. Hence the remote team can:
- Guide the bedside team through procedures
- Perform patient evaluations via HD two-way video sessions
- Order and interpret tests like MRI and bloodwork
- Order medications, order procedures such as intubations, extubations, central line placement (invasive line procedures), order restraints, etc.
- Run codes
A TechTarget article defining eICU explains that both teams discuss each case at the beginning of a shift and do an acuity assessment by classifying patients. (Note: Comparative acuity is often key for hospital performance evaluation – such as through the use of APACHE scoring.) The patient evaluation allows the onsite team to understand whether a more in-depth assessment is required of the tele-intensivist and prioritizes medical interventions.
Patients are classified as follows:
- Having multiple or numerous critical healthcare challenges
- Improving; can be moved out of the ICU such as to a step-down unit or to the medical floor
- Illness with an unclear acuity or trajectory, therefore, necessitating additional observation
Other electronic and digital devices:
- Connected video monitors, microphones, and two-way cameras
- Around the clock helpdesk to troubleshoot tech issues
- Dedicated secure phone lines
- Smart alarms
Key Takeaway
Medicine must embrace a combination of some of the most exciting new technologies, and several tech-inspired hospitals and clinics already have. However, this is merely scratching the surface of what’s possible. While Covid took healthcare into the future, the question remains how to maintain eICU interest and continued acceptance and adaptation in a post-pandemic world.
The bottom line is patient-centric: saving lives and improving patient outcomes and experience (including, when relevant, comfort care). The Hospital-Setting HCIA Evaluation; Final Third Annual Report provides a detailed meta-analysis and evaluation of the Health Care Innovation Awards. One finding that stands out regarding eICU and its benefits is:
“The eICU staff remotely monitored patients in participating ICUs via telemetry, and alerted clinicians at the bedside when they noticed any potentially problematic changes in patient vital signs that exceeded clinical guidelines. This monitoring was credited with numerous “saves” when problems were brought to the attention of bedside staff that might otherwise have gone undetected, endangering patient safety.”