DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
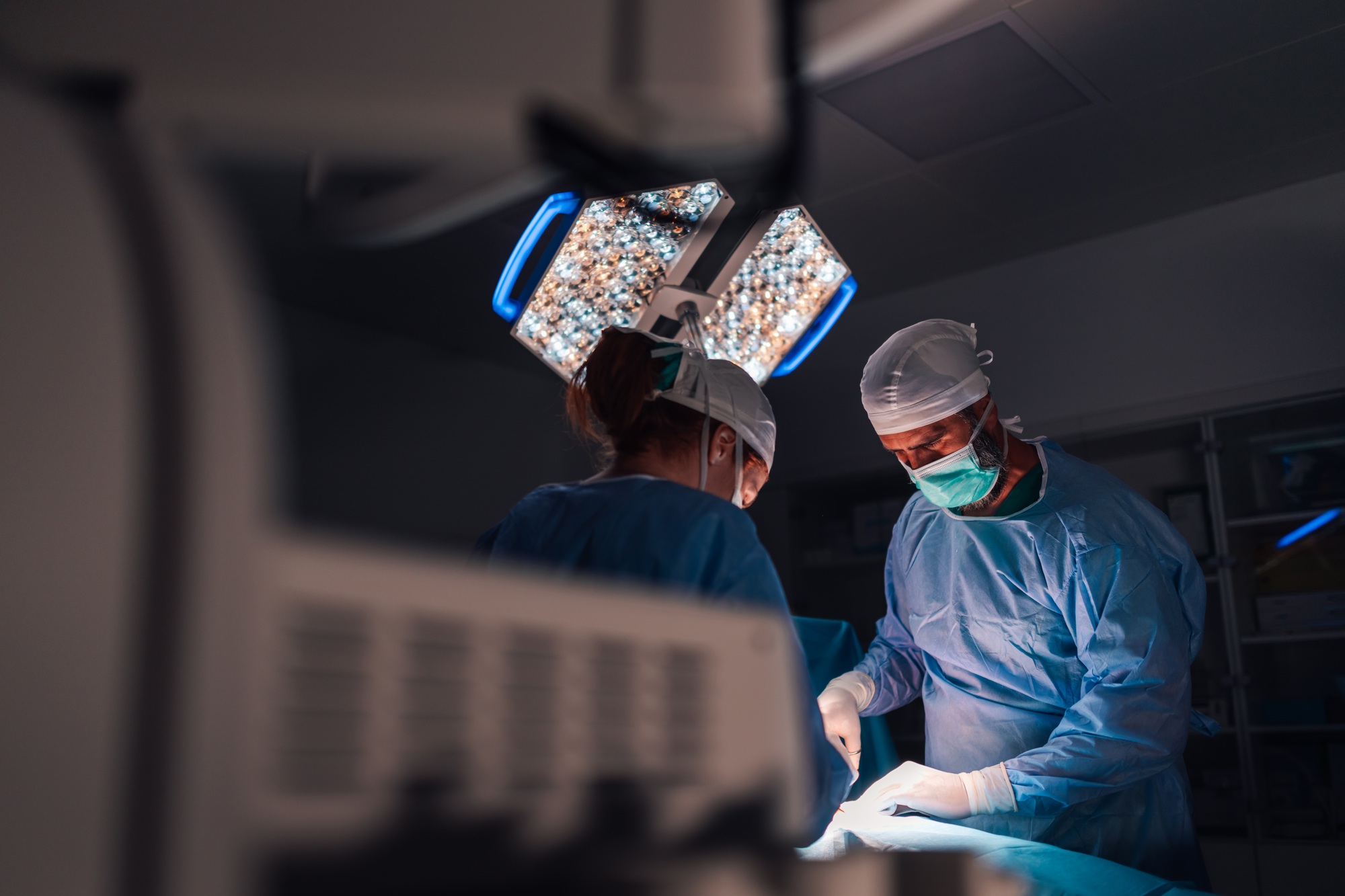
Hospitals across the nation have been creating Virtual ICUs to enhance patient outcomes in the intensive care unit. Since COVID-19, eICUs have proliferated – in one form or another — as healthcare facilities have focused on optimizing their resources.
Virtual ICUs employ registered nurses
Virtual ICUs employ registered nurses (RNs) with bedside critical care experience who use telemedicine technology as eICU RNs to remotely monitor patients and provide advice to their bedside nursing colleagues, and alert intensivists to something that has caught their attention during reviews. This additional ICU support has proven to be helpful, particularly given the shortages of critical care providers (especially intensivists and critical care RNs).
The COVID-19 pandemic has compounded the problem of staffing shortages, stressing already frustrated RNs to or beyond their breaking points. Nursing has always been a tough job. However, a 2021 study by Incredible Health found that more than a third (34%) of nurses surveyed said that they are very likely to quit their job by the end of 2022. Of these, 44% named a high-stress environment and burnout as the reasons. Also, pay and benefits were the second leading motivating factors (27%). In addition, the American Association of Critical-Care Nurses (AACN) reports that 66% of critical-care and acute nurses have contemplated quitting the profession altogether.
Having said that, what is it like to work as an eICU RN? What are the duties, and how does the Virtual ICU enhance patient outcomes?
What Is an eICU Nurse?
As a collaborative patient care team member, an eICU nurse provides telenursing care simultaneously to multiple critically ill patients who can be in different ICUs at distant hospitals. To deliver high-quality remote clinical services and ensure that each patient’s care plan is tailored to meet their needs, the eICU nurse works closely with hospital intensivists (board-certified critical care physicians), eICU intensivists, bedside nurses, and other multidisciplinary care team members. The eICU nurse reports directly to the operations director of the eICU program.
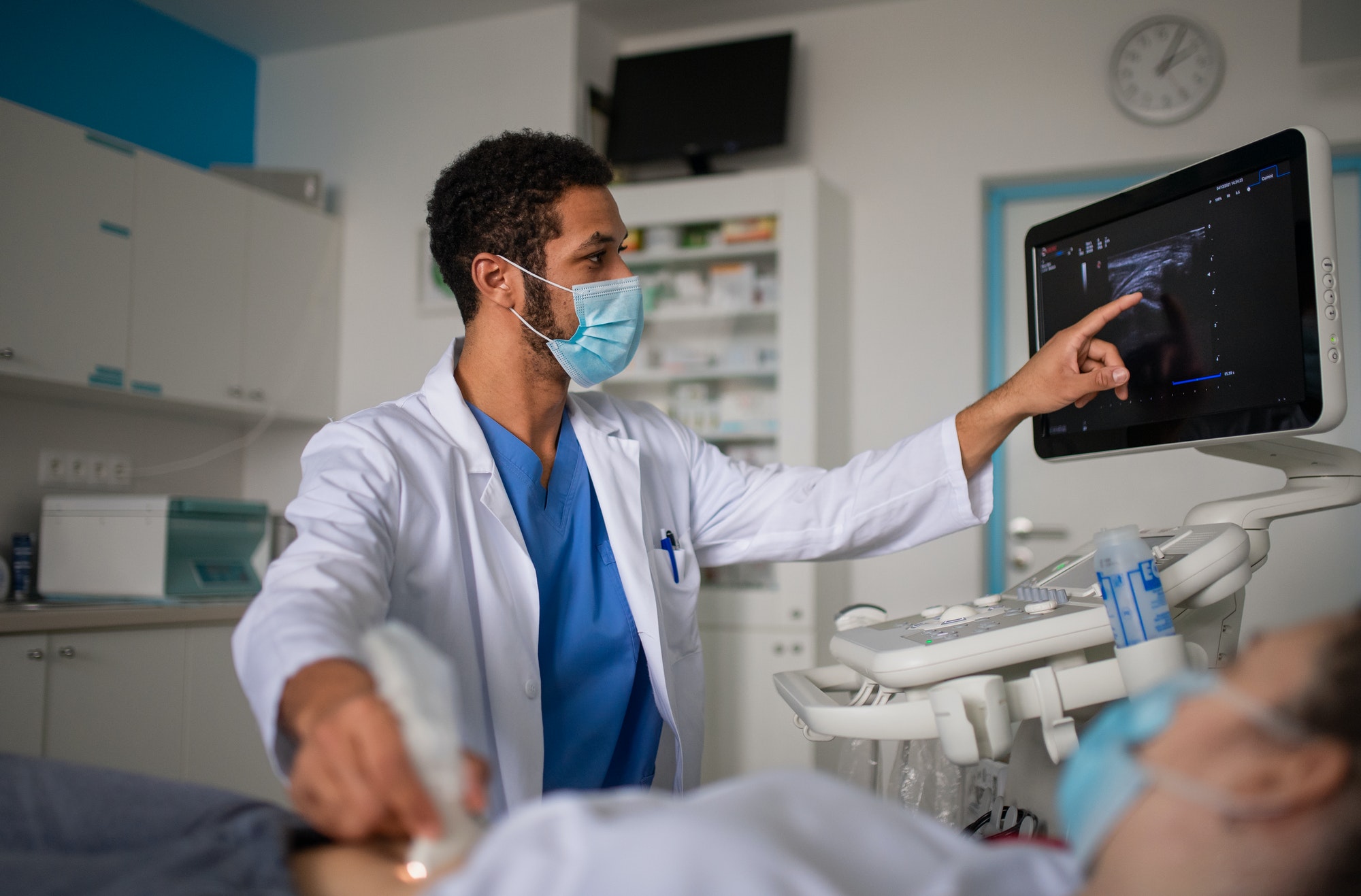
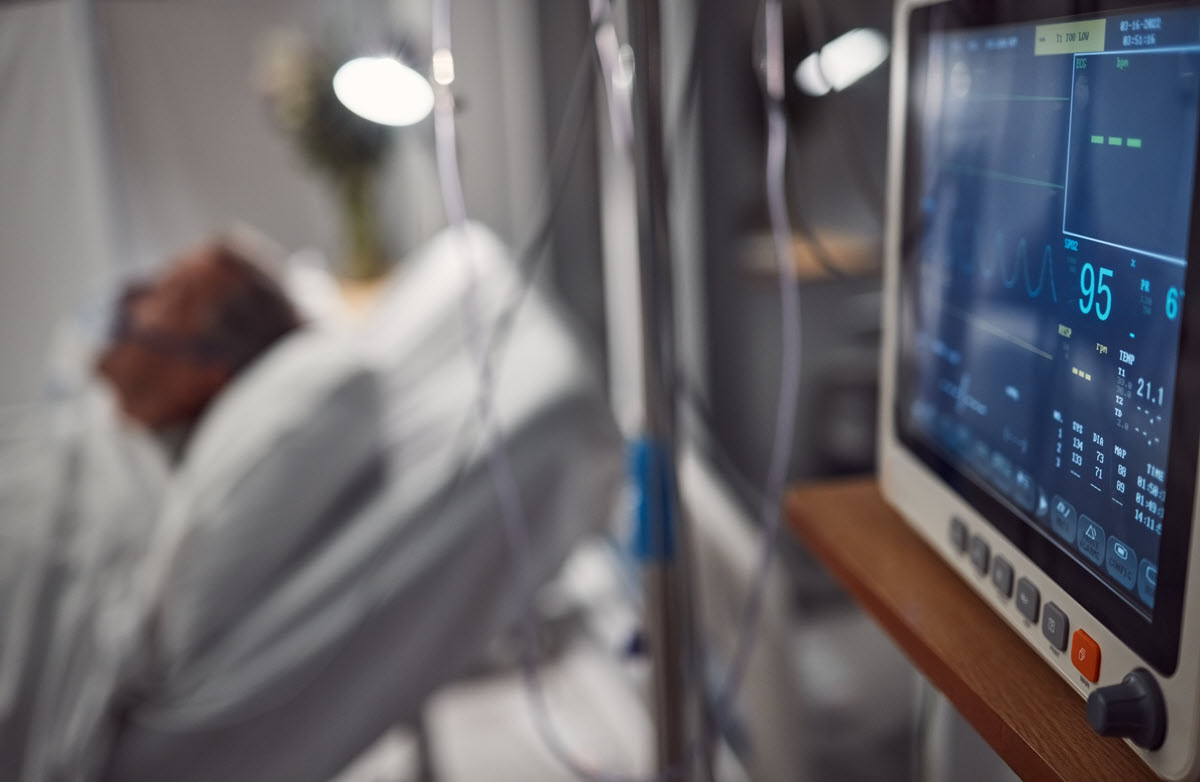
An eICU RN heavily relies on both communication technologies as well as clinical knowledge and experience. eICU nurses monitor each patient’s organ systems and vital signs using cutting-edge medical technology thereby supporting and aiding bedside teams.
Role and Responsibilities of an eICU Nurse
Critically ill patients may receive around-the-clock, immediate management from eICU nursing teams. Medical specialists, both RNs and physicians, perform real-time remote patient monitoring of ICU patients in support of bedside teams, including two-way audio-visual evaluations and alert bedside staff if necessary. The eICU team’s goal is to assist on-site caregivers in preventing patient deterioration or quickly stabilizing patients whose condition does worsen.
The following are typical roles and expectations of an eICU nurse:
- Provide off-site intensive care monitoring services:
Monitor critically ill patients and examine clinical data across several hospitals utilizing technology which assists in spotting patterns in patient data which might point to potential deterioration before it actually happens
- Foster collaborative partnerships and utilize clear and concise communication to support critical care staff, relying on their clinical experience/knowledge and interpersonal skills,.
- Exhibit excellent decision-making and problem-solving abilities.
- Protect patients’ privacy.
- Act as a patient advocate.
- Interact with the bedside ICU teams and members of the eICU center in order to facilitate delivery of safe, error-free care in routine and emergent situations.
- Troubleshoot clinical issues independently when appropriate and alert healthcare facility professionals about unresolved problems.
- Participate in clinical committees and quality initiatives.
eICU RN Qualifications
eICU RNs rely on extensive critical care expertise in order to successfully navigate the challenges of the job.
An eICU nurse typically has the following qualifications:
- Valid registered nursing license from the state where the patients are located.
- A Bachelor’s degree.
- The American Heart Association (AHA)’s latest Advanced Course in Life Support (ACLS) and Current Basic Life Support (BLS).
- CCRN certification and critical care nursing experience of at least three to five years.
Key Takeaway
In an eICU, critical care nurses and intensivists work off-site using advanced telemedicine technology. They can document and run advanced cardiac life support resuscitations and walk a patient’s on-site care team through complex bedside processes. They can communicate directly with patients and/or their families, including discussing difficult “end-of-life” decisions. Having these discussions can unburden the bedside nurses on whom this responsibility often falls (especially at night), thereby alleviating some of the pressures and feelings of guilt they might experience.
Hospitals and health organizations which have implemented teleICU solutions have seen remarkable benefits in patient outcomes, LOS, and access to health care (especially in outlying/rural areas). ICU staff at these institutions have also reaped the benefits of teleICU. These include stress reduction, graveyard shift coverage, assistance with patient monitoring, and performing tasks thereby freeing up staff to complete other work and tasks.