DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
During the COVID-19 pandemic, the US government waived many cross-state physician restrictions to increase and the availability of remote clinical care. The expanded implementation of eICU telemedicine proved invaluable during the pandemic, particularly for hospitals in outlying regions. However, the waivers are slated to expire as soon as the federal pandemic-era emergency order ends. Advocates of virtual care are seeking long-term policy changes to prevent this.
The Issue at Hand
Two years of the COVID-19 pandemic are behind us and the benefits of high-quality telemedicine, particularly in fields such as eICU, have become evident. However, the future of telemedicine will be significantly affected by the upcoming federal decisions regarding medical licensure. According to the medical licensing legislature, which dates back to the 19th century, doctors must be licensed to practice medicine in each state where they treat patients, even if they are licensed elsewhere. Licensure is state-determined. However, during the COVID-19 pandemic, the government relaxed the rules and gave the nation a taste of more-flexible cross-state licensing policies. These emergency-ordered policies facilitated remote patient monitoring and physician visits across state lines. However, as noted in an NBC June 19 news report, several states are rolling back the relaxed telehealth access rules, thereby, causing patients to lose access to healthcare providers. According to the Federation of State Medical Boards, in 2021, pandemic-era waivers facilitated remote physician visits in 26 states. However, there are only 12 remaining states with such waivers and even these are apparently going to be canceled in the near future.
Health Industry Reacts
As many states look to revamp their policies regarding inter-state healthcare, telemedicine proponents hope to capitalize on virtual care’s positive momentum by trying to shape a friendlier physician-licensing environment. Some groups want increased national adoption of agreements like the Interstate Medical Licensure Compact, which eases the process of physicians obtaining bulk licenses to practice in the 38 participating states. Others are lobbying for mutual licensure agreements between the states. Virtual patient care advocates also maintain that as states end their waivers or allow them to expire, millions of sick people will lose extended access to telehealth medical providers. They may be left with no choice but to drive long distances to be treated by out-of-state providers. Without the waivers, patients’ physical locations would have to be confirmed before providers could provide telehealth services.
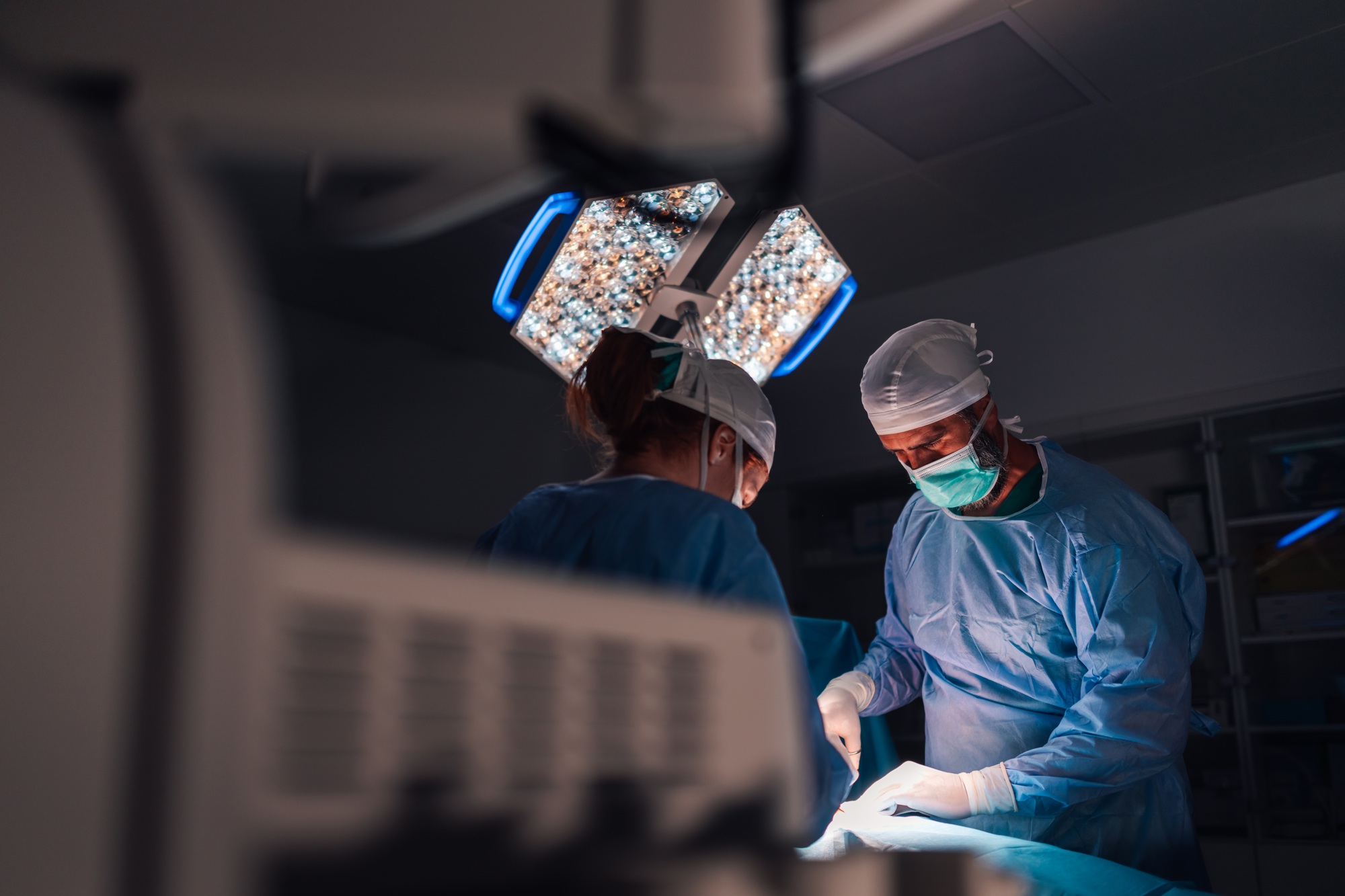
Impact on eICU
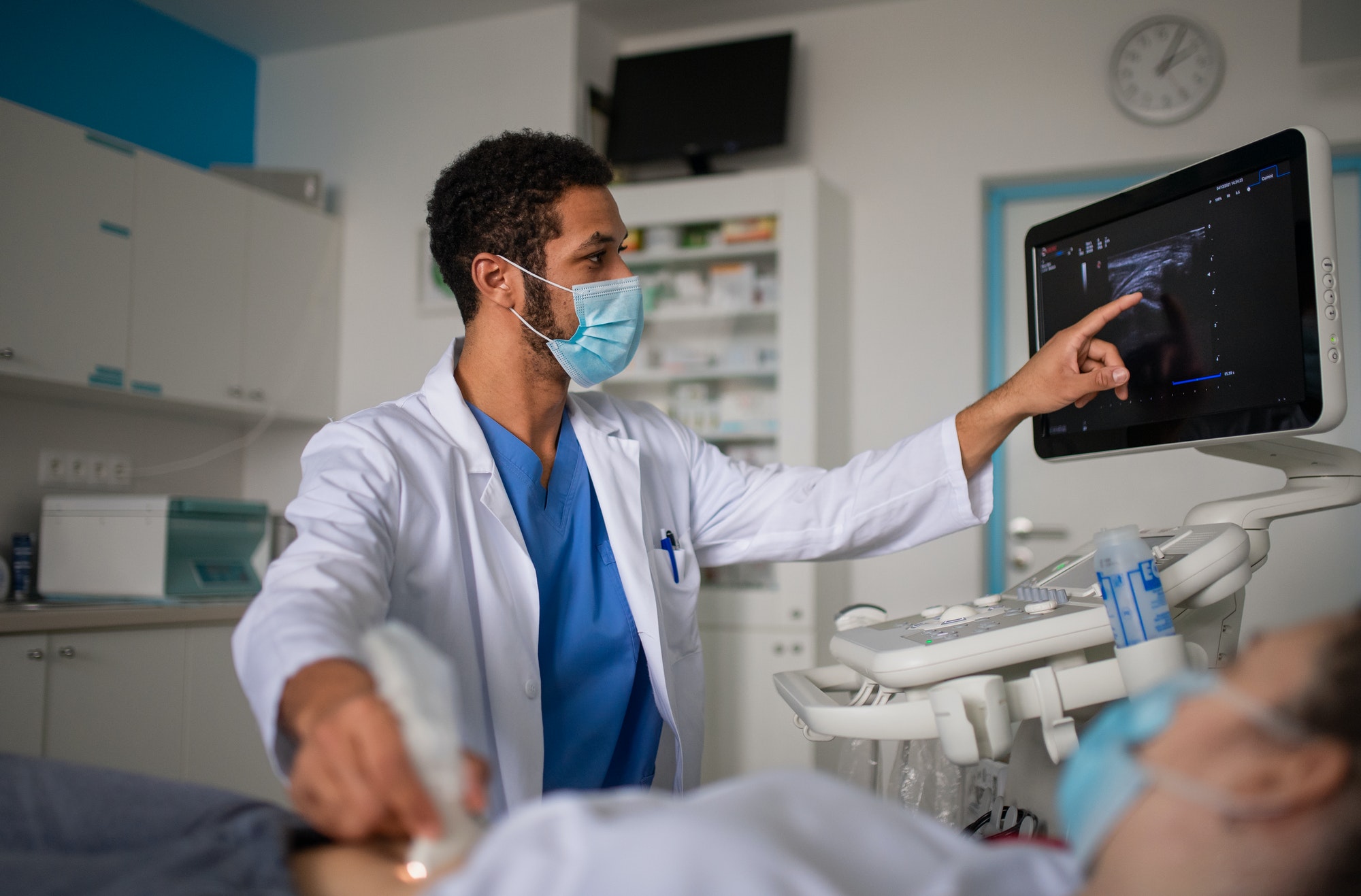
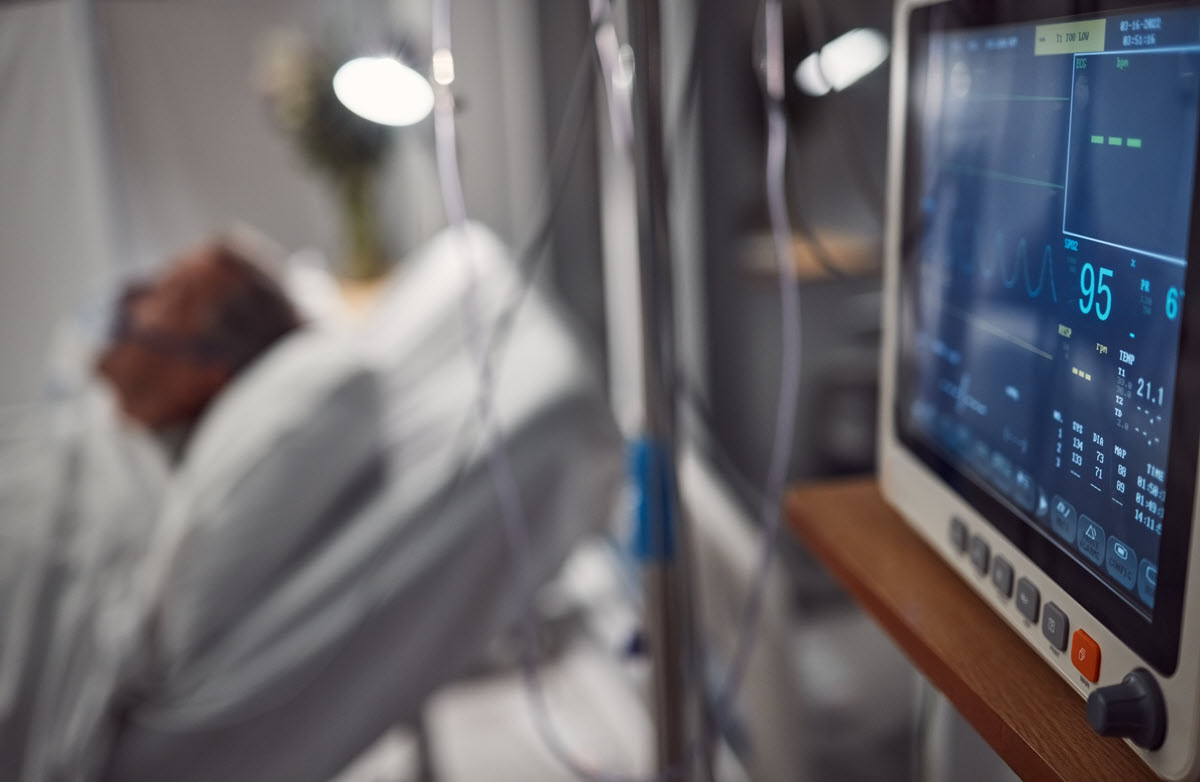
While surgery itself is a hands-on field, telemedicine and eICU have been critical in delivering preoperative consultations and preparations. The increased access to telemedicine technology enabled outlying hospitals, even those without an on-site physician, to retain and provide excellent care to critically ill patients rather than transferring them to other hospitals. Telehealth also alleviated problems related to the nationwide physician shortages in hospitals and particularly, in intensive care units. Additionally, telemedicine helped reduce hospital staff burnout – especially during the COVID-19 pandemic when medical staff were providing urgent care at the front lines. A return to pre-COVID rules and regulations would remove much of these benefits and might the future growth, development and implementation of telemedicine technology and services.
In the Balance
The US public health emergency declaration was scheduled to expire at the end of July; however, Congress recently extended the COVID-19 telehealth waivers for an additional five months. Furthermore, US Health and Human Services (HHS) plans to issue an extension and has stated that it will give 60 days notice before allowing the waiver to expire.
With the support of the California Medical Association (CMA), private and public health plans extended their coverage and reimbursement for telemedicine services during the COVID-19 pandemic. The CMA has also published a Telehealth Policy Update summarizing current federal and state legislator decisions that will shape the future of telemedicine this year and in years to come. Meanwhile, the public health crisis continues and all of the aforementioned policies remain in effect.