DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
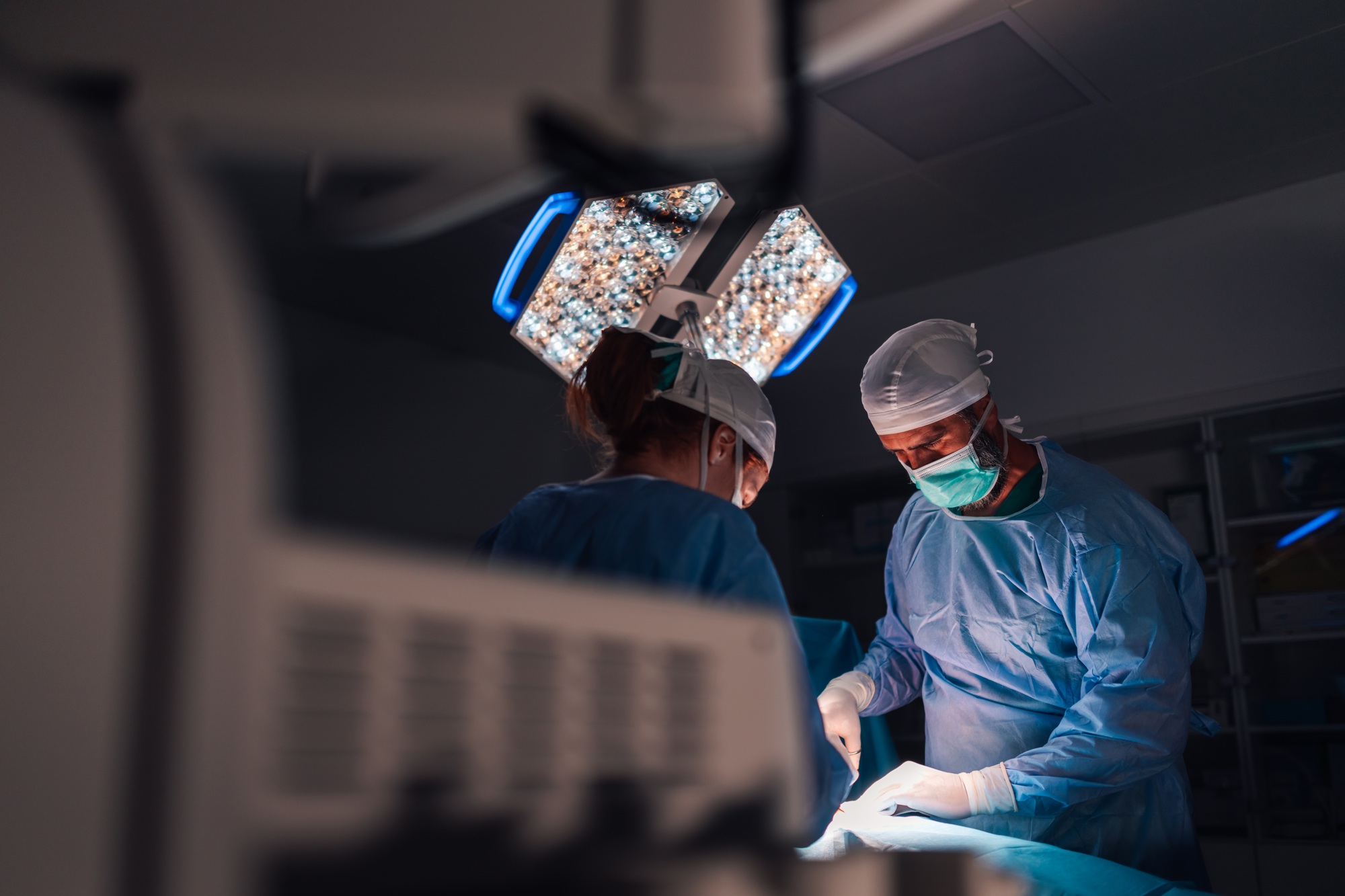
Over 5 million patients are admitted to the ICU every year in the United States. Of these, the average patient stays in the ICU for around 3.8 days, depending on the nature and severity of his or her condition. As no one wants to spend time in the hospital, least of all in a critical care ward, it is important to ensure that the patient experience is as comfortable and positive as possible.
The patient experience itself refers to the patients’ (and/or the family’s) perception of their overall experience during their medical treatment. This includes patients’ encounters and interactions with doctors, nurses, and other staff; the hospital admissions process; wait times; communication throughout the stay; patient safety; level of comfort, and more.
While it is up to the patient to express his or her own feelings as to what their hospital – or more specifically, ICU – experience was like, there are certain elements that are generally key to the evaluation. These elements include: access to doctors, communication, decision-making, and overall outcome (including length of stay and mortality rate).
eICU can improve patient experience
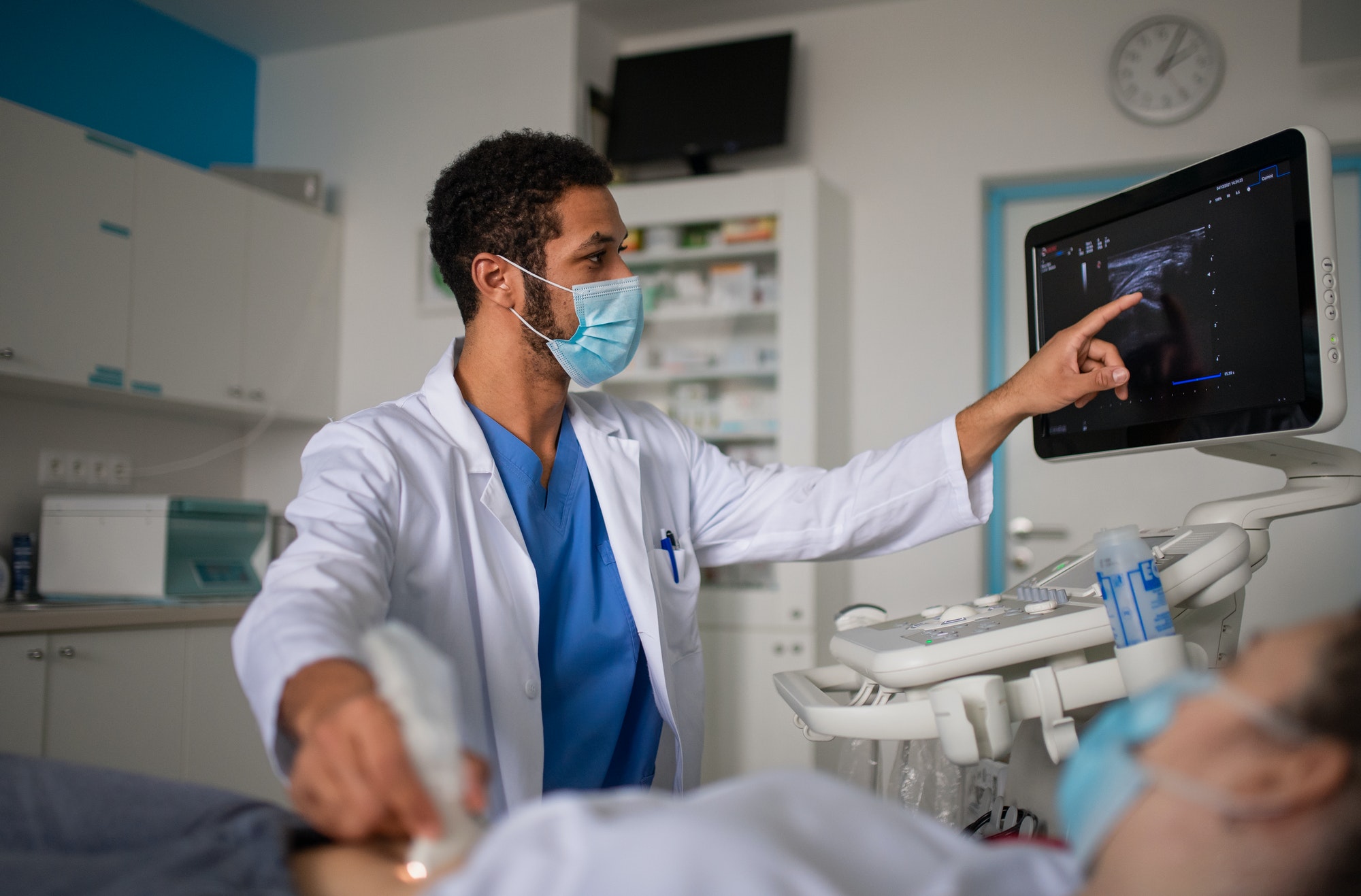
The introduction of an eICU can improve the patient experience in all four areas. As telehealth visits and virtual visits with doctors become more commonplace outside of the ICU, patients and family members alike will continue to grow more and more comfortable with the idea of a remote doctor being heavily involved in patient care, even in a critical care setting.
How Does Telemedicine Improve Patient Experience?
Access to Higher Quality Doctors
The entire medical industry is experiencing a shortage of doctors across the board, and critical care is no exception. Up to 47% of surveyed healthcare workers in the United States plan to leave the field by 2025. The shortage of medical professionals will leave many critically ill patients without access to high quality ICU care. The situation is especially challenging in rural areas and places where the hospitals don’t have the funding to attract the most well-trained and talented intensivists.
Unfortunately, many patients and families are put in the position of having to choose whether to try their luck at a local hospital, where the patient care may be sub-par, or agreeing to transport the patient. The transportation itself can be costly and, depending on the patient’s condition, risky, to say nothing of the inconvenience and additional challenges it adds on a family if the patient is in the hospital for an extended period of time very far from home.
Integrating an eICU is a cost-effective way for a hospital to admit more patients and give them access to top critical care physicians, even if they are in a remote location. These doctors are able to use telecommunication technology to provide the on-site doctors with the additional support they need to be able to treat the patients effectively.
Better Communication
One of the biggest complaints that patients and family members have about their hospital stays hasto do with communication with their medical practitioners, or the lack thereof. Because the doctors and nurses in the ICU tend to be overworked and overwhelmed, they do not always have as much time as they would like to talk to patients. Patients and their families are then left scrambling for answers to their questions.
Without accurate and updated information on the patient’s condition and prognosis, both the patient and the family may feel in the dark and confused about what to expect or what the next steps should be. This uncertainty can add an extra layer of stress to an already unpleasant situation. For example, family members need to know as soon as possible if they should be looking for long-term rehabilitative care for the critically ill patient so that this doesn’t come as a surprise as they are being released from the hospital.
With an eICU, there is an additional layer of support for the patients. Even in cases where the remote doctors are not in direct contact with the patients themselves (but rather are monitoring vital signs and other key indicators), the pressure they take off the on-site doctors will allow those physicians to devote more time to the patients in order to explain the situation and the plan of care.
More Effective Decision-Making
Management of a critically ill patient in the ICU is a dynamic process which requires frequent decision-making. Based on the patient’s condition and vital signs, medication or treatment protocol changes may be warranted. Decisions will also need to be made regarding release from the hospital or, unfortunately, on issues relating to hospice or end-of-life care. These decisions are usually made in consultation with the patient and/or family members and should not be taken lightly.
The shortage of health care personnel and the resultant overwhelming of care providers often leads to important decisions being made too quickly without proper evaluation or without input from the family. Or even worse, some issues may fall through the cracks entirely, putting the patient’s safety at risk.
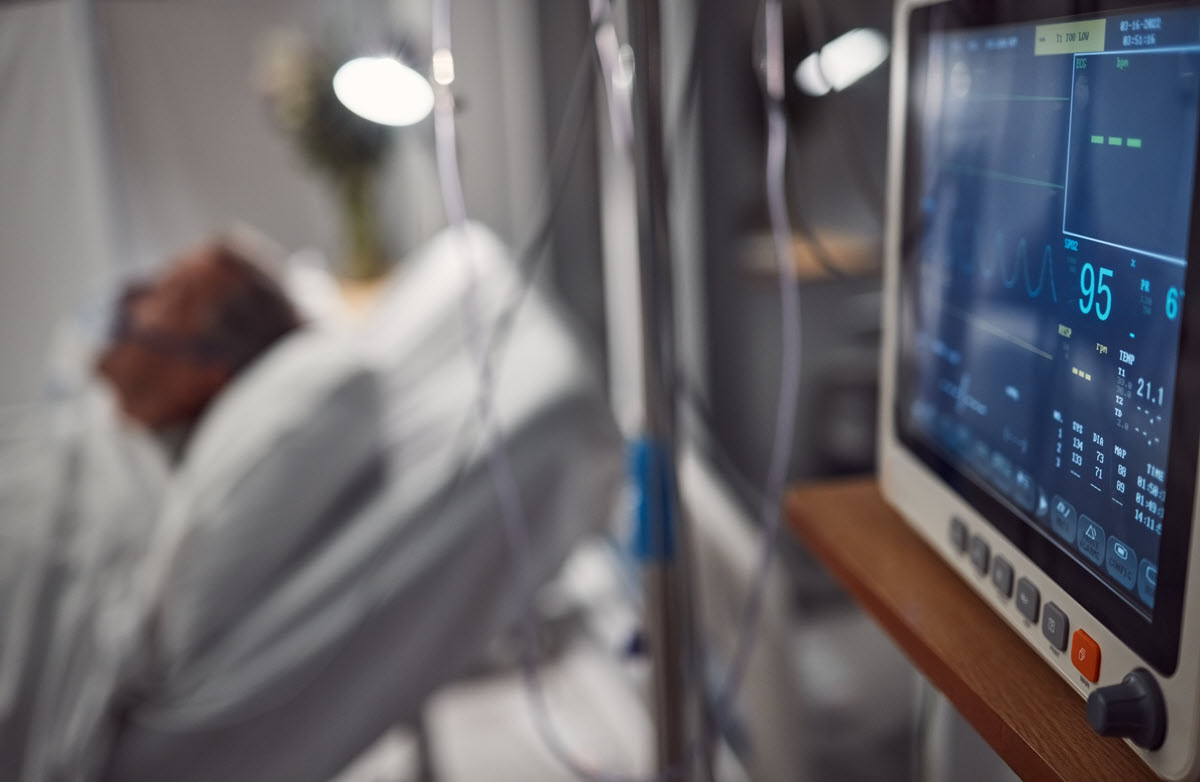
When a patient is being monitored remotely 24/7, the remote staff can flag any unexpected changes in their vital signs and can contact the on-site doctor and direct them to where their focus is most needed. Having more “hands on deck” enables the collection of more information that can be used to make the best and most effective decisions.
Improved Patient Outcomes
Of course, the best possible outcome is the return home of a healthy patient. Studies over the last decade have consistently shown that the implementation of an eICU into a hospital’s intensive care unit improves patient outcomes. There is widespread agreement that eICUs lead to a decrease in mortality rates and also decrease the amount of time patients spend in the ICU.
There is no question that the access to remote doctors and the pressure that this alleviates for the providers at the bedside enables patients to receive better and more effective care, resulting in better outcomes. These benefits have a ripple effect because the more quickly patients are able to recover and leave the ICU, the more space there is for new patients to come in.
eICU Improves Patient Experience
Since the passage of the Patient Protection and Affordable Care Act in 2010, hospitals have made improving patient experience a priority across the board. Integrating a telehealth service such as a remote ICU can go a long way to improve patient satisfaction and quality of care, especially for hospitals with limited critical care staff and an overload of intensive care patients.