DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
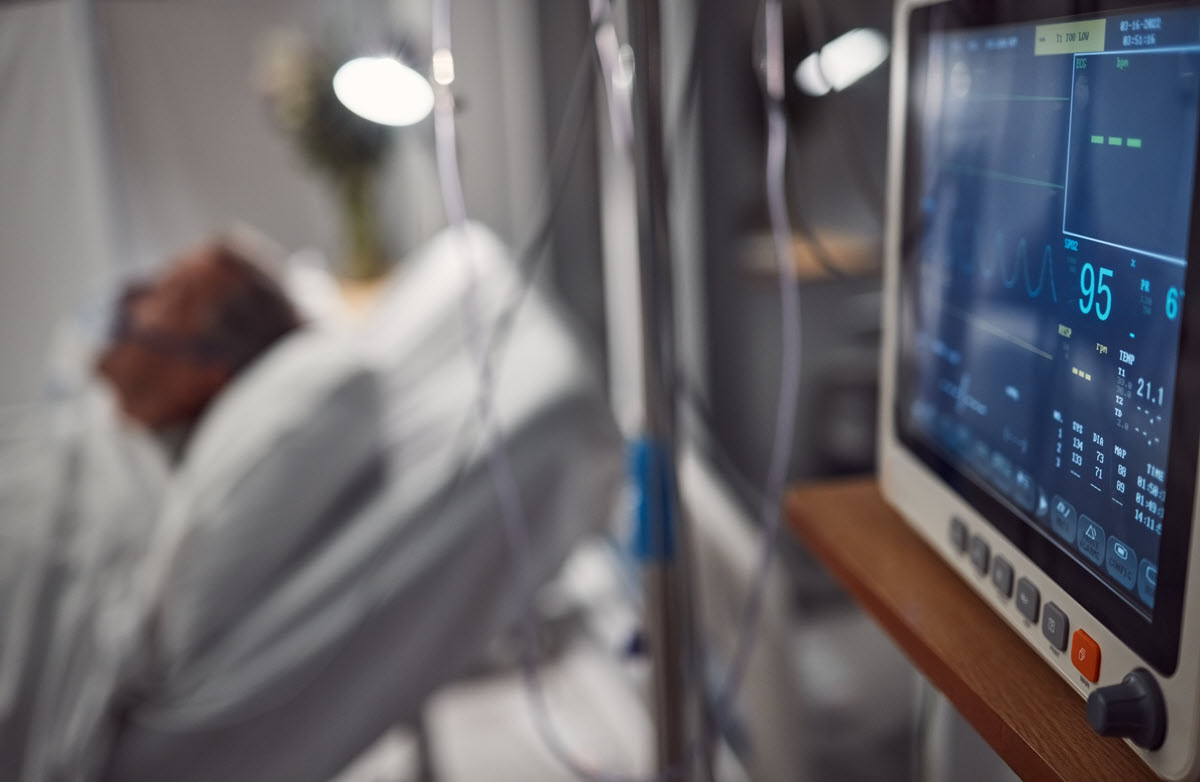
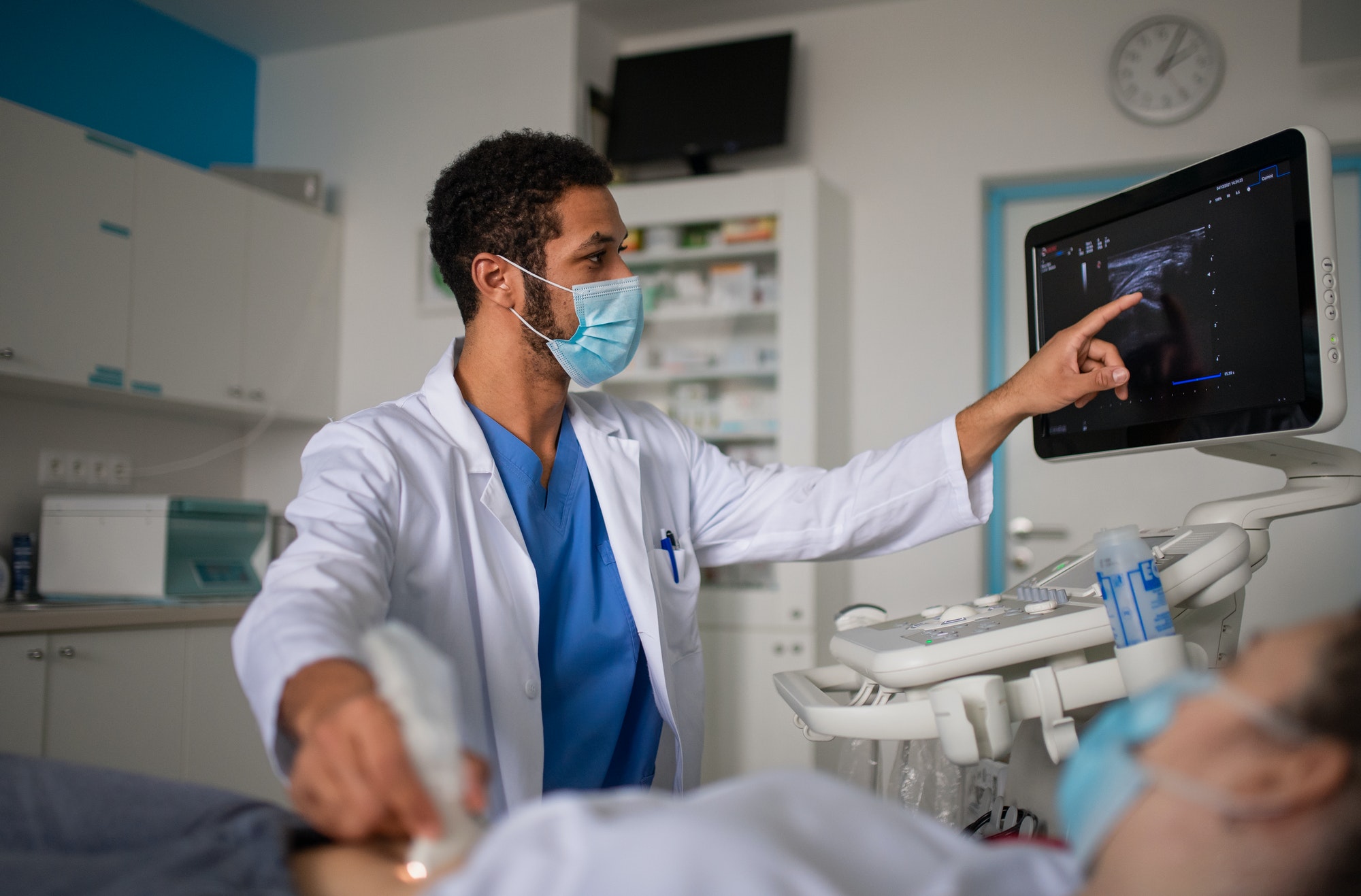
The use of tele-ICU services has grown rapidly in recent years as hospitals seek ways to leverage technology to improve care quality and patient outcomes. Tele-ICUs allow offsite critical care teams to monitor ICU patients remotely using audio, video, and data feeds. This enables round-the-clock coverage and early intervention when patients show signs of deterioration.
When implementing a tele-ICU program, hospitals must decide whether they want to implement a proactive or reactive approach to patient management.
With a proactive tele-ICU, the remote critical care team takes a hands-on role in patient care, making recommendations and intervening at the first sign of decline. They analyze real-time data to anticipate problems and suggest preventive therapies to the bedside team. The goal is to get ahead of complications and avoid adverse events.
Reactive tele-ICU model
In a reactive tele-ICU model, the offsite team acts more as a safety net, intervening only after a patient has started to deteriorate. They offer support upon request but otherwise let the bedside ICU staff direct care. This approach aims to leverage technology to identify emergencies and urgent needs.
Proactive tele-ICUs have been associated with reduced ICU mortality rates, shorter lengths of stay, and fewer adverse events like sepsis and cardiac arrests. However, they require significant investment in staffing and technology and a willingness to change bedside culture and workflows. Reactive programs may provide more moderate benefits but facilitate an easier transition for on-site clinicians.
Overall, evidence suggests that proactive tele-ICUs enable earlier interventions and better outcomes. But the right approach depends on hospital resources and goals. Thoughtful implementation is key to maximize the value of remote critical care services.
Preventing Adverse Events with Proactive Tele-ICU Care
Critically ill ICU patients are at high risk for adverse events like sepsis, pulmonary failure, and cardiac arrest. Studies show that between 30-70% of such events may be preventable with timely intervention and care process improvements. Tele-ICUs can play a pivotal role in proactively identifying risks and preventing complications through round-the-clock monitoring and clinician support.
Some ways a proactive tele-ICU approach can help avoid adverse events include:
- Analyzing real-time vitals, labs, and alarms to detect subtle signs of deterioration that might be missed at the bedside. Early interventions can prevent further decline.
- Reviewing infusions, medications, and recent orders to anticipate patient responses and possible unintended consequences. Dose adjustments may be recommended.
- Monitoring culture and lab results and recommending tailored antibiotic therapy to reduce sepsis risk.
- Ensuring best practice protocols are followed for ventilator weaning, sedation, thrombosis prevention, and other aspects of care.
- Performing safety surveillance to reduce risks like hospital-acquired infections and pressure injuries.
- Communicating risks and recommending preventive steps to bedside teams through timely call-outs.
With its expansive data capabilities and clinical expertise, a proactive tele-critical care program is uniquely positioned to recognize threats, improve compliance, standardize care, and help bedside teams avoid preventable harm. This can lead to significant improvements in quality of care and patient outcomes.