DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
The development of technology for healthcare is a natural evolution in the digitized world. Telemedicine, delivering healthcare by remote technologies, is not a new concept, but COVID-19 pushed it — and particularly eICU — into the forefront as the safest feasible method for doctors and patients to interact. In addition, telehealth resolved issues with in-person appointments such as social distancing rules and transportation limitations. Overall, in a time of great need, telemedicine unequivocally demonstrated and proved not just to skeptics but to society at large how it augments healthcare access for isolated individuals in a variety of settings. Moreover, the success opened many eyes to the possibility of additional benefits. One such potential benefit is the use of remote language experts, medical translators and interpreters, bridge language and cultural gaps, thereby allowing equal access to care.
Recognizing technological and language barriers
One may ask why has telemedicine not yet addressed language barriers as part of its technology, for example, by incorporating translation software? By and large, technology develops with and in response to emerging needs. Progress does not occur overnight but evolves as specific situations arise, which are then naturally given precedence over others. In our example, telemedicine’s demonstrated abilities in action during the COVID-19 pandemic enabled many in the industry, including those who had previously discounted it, to see its benefits and to understand its future investment-worthy uses.
A significant portion of the population is not tech-savvy
For instance, a significant portion of the population is not tech-savvy, especially the elderly. It is the elderly who are the fastest-growing population group and who stand to benefit most from telehealth. Distinguishing between inpatient and outpatient medicine is important in this context, as, for example “users” or “end users” – if one may think of patients that way for a significant portion of telemedicine – would typically be patients who are not admitted into the hospital, so outpatients. So in a vICU or virtual ICU or TeleICU setting whereas a significant portion of the patient census may be elderly, whether they are tech-savvy or not is immaterial for them to reap major benefits from their presence in an eICU-enabled critical care unit in a hospital. This is due to the end-users of the telehealth in place in the SICU, MICU, CVICU, CICU, or Tele-ECMO (i.e., electronically monitored surgical ICU, medical ICU, cardiovascular ICU, heart-lung machine, etc.) are trained hospital intensive care unit staff and obviously the Tele-critical care specialist physicians, TeleICU nurses, and other clinical staff on the remote monitoring side of the camera, i.e., “in the bunker” or “in the COR” or “in the hub,” as it were.
Outpatient medicine
Returning to outpatient medicine (when patients are not admitted into the hospital, for generally less acute matters), many potential recipients of at-home consultations or other remote healthcare may be unable to use the services due to the lack of the required technology in their homes or their inability to use it even when they have it. This could also be true for individuals who do not have sufficient English skills to understand the instructions on how to use the technology.
An article by PolicyLab, the Children’s Hospital of Philadelphia (CHOP) Research Institute, tackles “How Health Systems Can Help Address Language Barriers to Achieve Digital Health Equity.” According to the researchers, there is growing evidence that telemedicine’s benefits are not realized equally due to a digital divide. This is especially true for “historically marginalized populations, racial and ethnic minority groups, refugee and migrant populations, patients with Emerging English Proficiency (EEP), patients in rural areas, and individuals with disabilities.” Furthermore, the article states that healthcare systems and technologies designed for English speakers exacerbate the problem.
The problem is substantial given that US Census Bureau statistics show that presently, 9% of the US population (over 25 million people) have Limited English Proficiency (LEP). The national average of non-English speakers is 21.9%. 16% of US children have at least one LEP parent. This situation impacts telemedicine access. However, there are solutions.
A December 2021 research article published by the MDPI Journal discusses educating clinicians to improve telemedicine access for patients with LEP. Although the COVID-19 pandemic triggered the rapid implementation of telemedicine into healthcare systems, it augmented access inequities for US patients with LEP or no English. For instance, patients with LEP or no English have difficulty entering online portals and accessing electronic health (EHR) information. The COVID-19 pandemic also made access to qualified medical interpreters more difficult.
In the hospital ICU setting
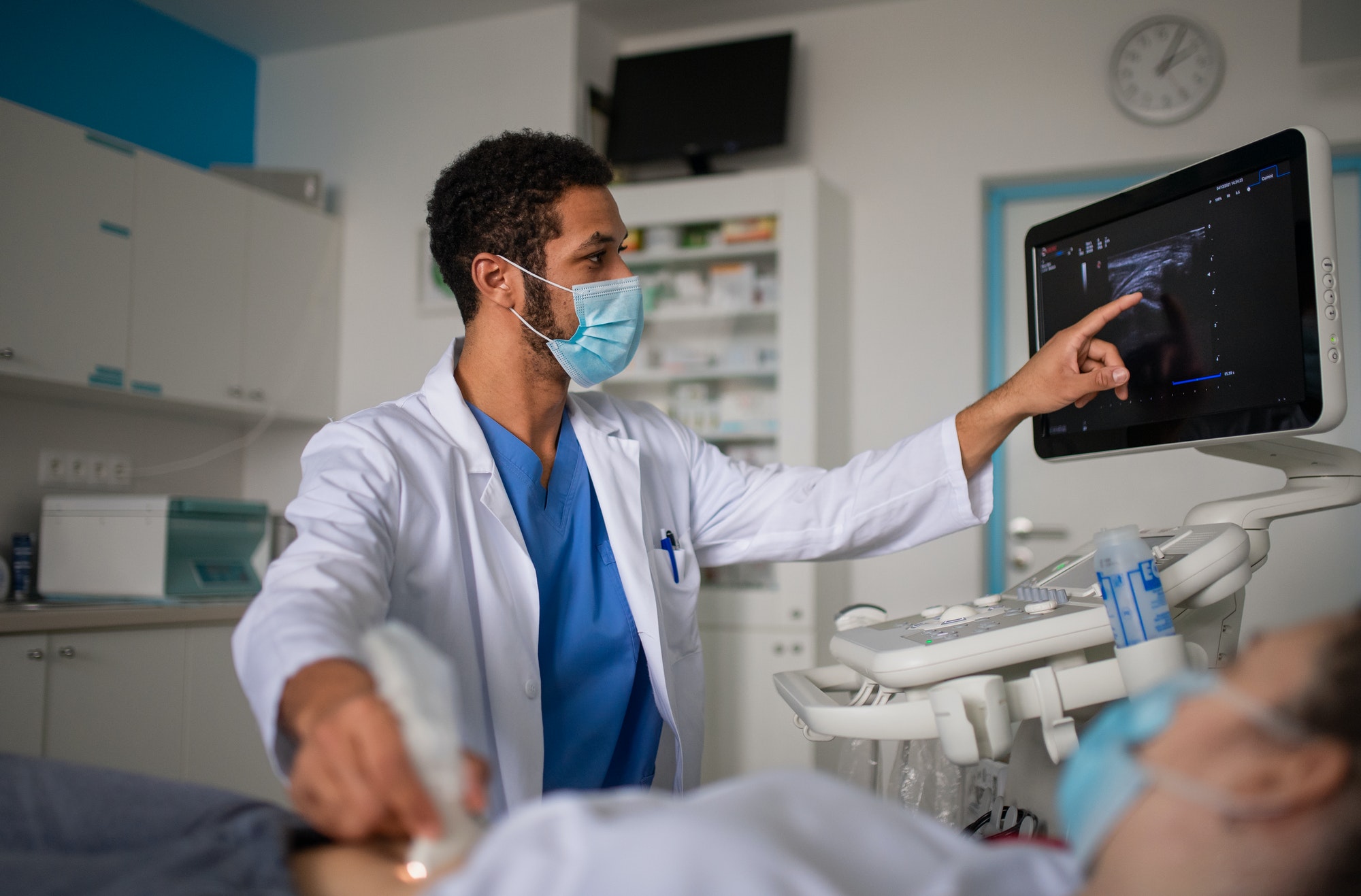
In the hospital ICU setting, communication between practitioners and patients (or their families) is critical. There have been cases where non-English speakers have been misunderstood and therefore misdiagnosed and/or incorrectly treated, with dire outcomes. Medical care is often time-critical, and translators may not always be immediately available. Hiring and having available providers who understand and speak the multitudinous languages of the world is impractical, if not impossible. The book Telemedicine in the ICU (Springer) proposes electronically connecting the physician and the patient (or the patient’s family) with a HIPAA-compliant medical translation service during e-ICU or tele-ICU interactions. During the COVID-19 pandemic, eICU intensivists were often patients’ first point of contact. Since many of the patients had LEP or were non-English speakers, this would have been a perfect solution to the communication problem.
Future mitigation
Countless articles have stated that telemedicine will continue to flourish post-COVID, given how it has proven its efficacy in the field during the crisis. Yet, as with all technology, there is room for improvement. Telemedicine and its specializations / specialties, such as tele-ICU, are technically advanced enough to step up to the plate by addressing issues that have come to the forefront and making the appropriate adjustments.
Providing equal access to care for linguistic minorities requires several measures. Such measures may include clinician training on how to work alongside interpreters, investing in innovative multilingual digital health technology, and allotting funds for multilingual digital health support.
Three overlapping obstacles to patients’ telehealth access
An article published by the peer-reviewed online journal Health Affairs identifies the three overlapping obstacles to patients’ telehealth access: lack of technology; unreliable internet coverage; and digital illiteracy. This digital divide “affects older people of color and those with low socioeconomic status,” which data show, are also at increased health risk due to COVID-19. The gap increased when COVID-19 forced doctors to close outpatient clinics and to instead, offer care from home using digital technology such as smartphones or computer video. It’s not just the elderly who are affected. According to the US Department of Education, 52 percent of adults who own a computer do not know how to use it correctly. Thus, during the COVID-19 pandemic, many people were unable to access the patient portals needed for these physician-patient encounters.
The article recommends that public health officers, community leaders, policymakers, and national decision-makers address the divide. For example, states are working to identify needy communities and distribute computers and other technology, such as smart-phones, often acquired from donations.
In conclusion, to quote the PolicyLab authors, “linguistically appropriate and accessible virtual care should be a priority, both now and after the COVID-19 pandemic subsides.”