DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
The disparity between ICUs with and without board-certified intensivists in the US is widening. This problem impacts the entire medical services ecosystem, from patients to doctors and hospitals. The problem is compounded by increasing ICU admissions, the expense of hiring full-time intensivists onsite, a lack of full-time critical care doctors, and other factors. However, the impact of TeleICU implementation has expanded the boundaries of critical care medicine and has worked toward alleviating the disparity among ICUs.
Shortage of Intensivists in Numbers
Many hospitals struggle to provide consistent ICU care due to a national shortage of intensivists, uneven distribution across metropolitan and rural areas, and a growing aging population. In addition, the COVID-19 epidemic has seen some hospitals – and even some cities or regions – with all ICUs beds occupied at certain times.
A research article published in 2013 on PubMed Central (PMC) stated that the shortage of intensivists in the US and the demand for them would only increase over time. According to an AHA survey, as of 2020, there were 6,146 hospitals in the US, 36,241,815 patient admissions, and only 5,500 board-certified intensivists. In addition, only approximately 35% of ICUs can provide intensivist care meeting the standard of care.
Effect on Patients
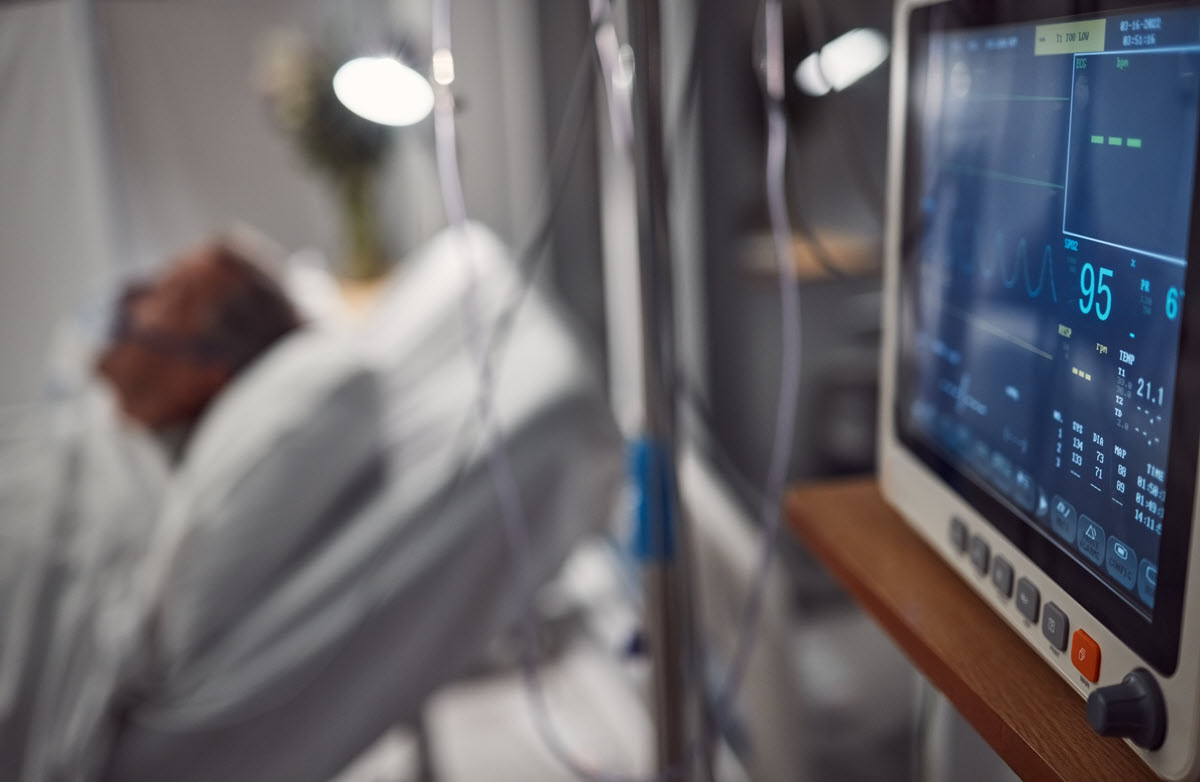
The effect on patients is palpable. Between 4 to 7 million patients are admitted annually to US ICUs for comprehensive management of injury and illness; intensive or invasive monitoring; stabilization of acute or life-threatening medical problems; support of airway, breathing, or circulation; and maximization of comfort for dying patients.
ICU patients are heterogeneous, but all need frequent assessment and a greater need for clinical and technologically-enhanced clinical support than patients admitted to non-ICU beds. Also, mortality in the ICU is extraordinarily high — nearly 1,500 people die after admission to an ICU daily in a pre-Covid environment, and almost one in five would succumb to their illness or injury in an ICU. Of course, during a pandemic such as Covid-19, those numbers can be far worse.
Research shows that when ICU patients are cared for by intensivists available around the clock, ICU mortality decreases considerably – indeed by as much as 40%.
In addition, healthcare-associated infections (HAIs) decrease, as do ICU costs and lengths of stay (LOS), the latter inevitably impacting the former. Hence the clear need for more critical care doctors the need to expand the coverage footprint of in a clinically-safe and effective and responsible manner.
In 2019 a clinical survey reviewed 2,814 acute care hospitals with 540,668 hospital beds, including 94,837 were ICU beds. The results showed that 1,345 (48%) had no intensivists, and 1,469 (52%) had intensivists. Those with intensivists had significantly more hospital beds (x2.9), ICU beds (x3.6), and a higher ratio of ICU to hospital beds. In aggregate, 78% of the total ICU beds are in hospitals with hospital-privileged intensivists.
Benefits of TeleICU for patients
By definition of an Intensive Care Unit, patients admitted need life-saving intervention and, for the most part, their survival is in the hands of the ICU team. Unfortunately, as the data above indicates, patients are at the most significant risk due to the fast-growing low intensivist/patient ratio. Overall, the situation reveals that the entire medical services ecosystem would benefit from a solution to this problem.
Research points to TeleICU implementation as one workable solution to the problem by leveraging modern technologies, especially given the complexity of today’s ICU services. In a digital age where technology is solving problems and enhancing efficiency across numerous industries, critical care should also be included.
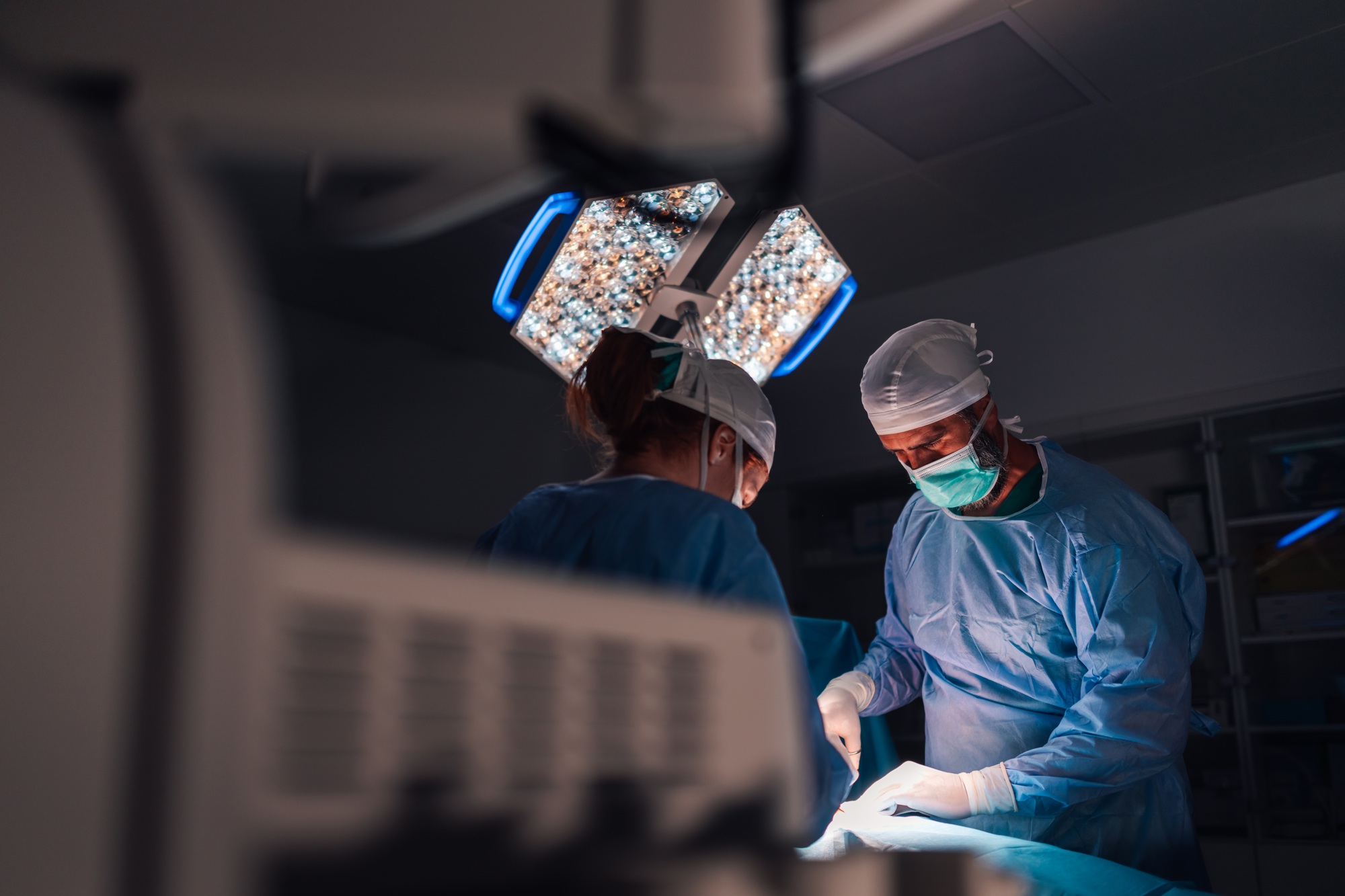
Command center with a 24/7 critical care team
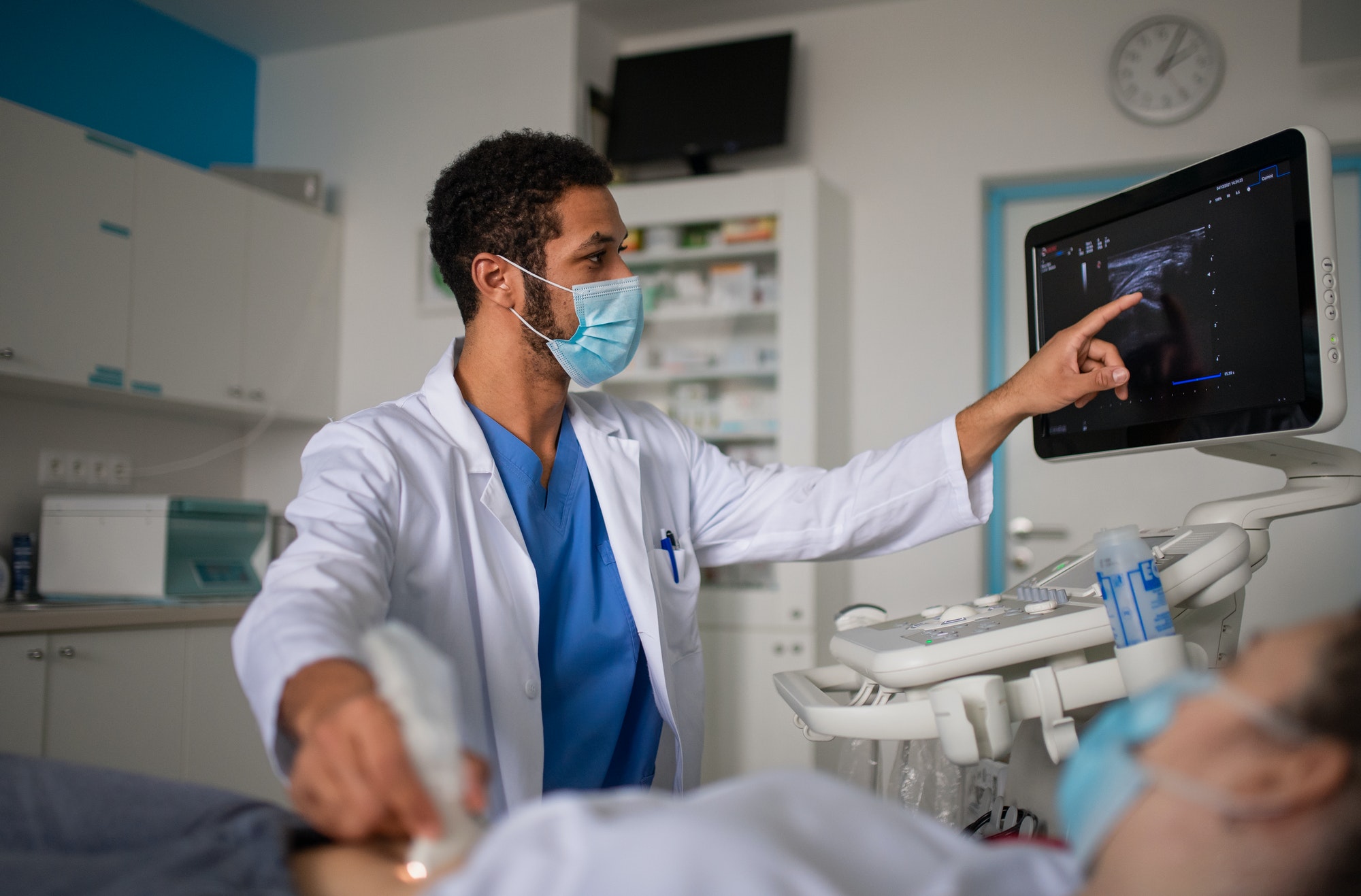
A TeleICU off-site command center with a 24/7 critical care team (intensivists and, sometimes, critical care nurses to support the intensivists’ work) can connect patients in distant ICUs through real-time audio, visual and other electronic means including direct access to the patient’s electronic medical record (electronic chart, EMR). Like a bedside team, off-site TeleICU intensivists require full access to the patient’s data available to the clinical team in the physical ICU. This method brings a Tele-intensivist straight to the patient regardless of their location.
Tele-critical care helps particularly remote or small ICUs – but also even larger or more urban-located ICUs — with no full-time intensivists by preventing patient transferals delaying urgent, life-saving treatment. In addition, the solution helps ICUs with overwhelmed critical care physicians working at the patient bedside suffering burnout (to be investigated in Part 2 of this article). It accomplishes this in many ways, including providing real-time monitoring of patient instability or any abnormality, ordering diagnostics tests, making diagnoses and ordering prescriptions and procedures to be placed on the patient, and implementing any appropriate intervention through controlling life support devices.
As a result, telehealth ICU holds great promise in enhancing the quality of critical care patients and increasing the productivity of intensivists. Tele-critical care physicians can improve mortality and LOS due to:
- Critical care physician case review within one hour of admission
- Timely use of performance data by management
- Adherence to ICU best practices by tele-intensivists and bedside team
- Quicker alert response times among all clinicians
- Alleviating staff shortages, workload, and burnout which can harm patient outcomes
- Substituting NPs and PAs with physicians
TeleICU implementation continues to grow in the US, with 18% of adult ICU beds already covered by TeleICU. It warrants emphasizing that with the patient being the focus, the ripple effect of TeleICU technology improves the entire medical services ecosystem. This improvement includes addressing the problems of board-certified intensivists, their teams, and the hospital in general.
Read part #2 >>>