DISCLAIMER: The below blog entry was written by an outside, unrelated party and does not necessarily express the opinions or views of or associated with the RemoteICU brand or the individuals associated with the RemoteICU brand. The blog is not necessarily endorsed or supported by RemoteICU nor was the entry reviewed and accepted by individuals associated with RemoteICU. The blog entry is provided simply to address and create interest in topics of import related to telemedicine. Your own independent research and decision-making and seeking of expert / professional opinions are required before you make any decisions whatsoever or form any opinions with respect to any topics addressed therein. By reading the blog entry, you consent to accepting the terms and conditions in this disclaimer.
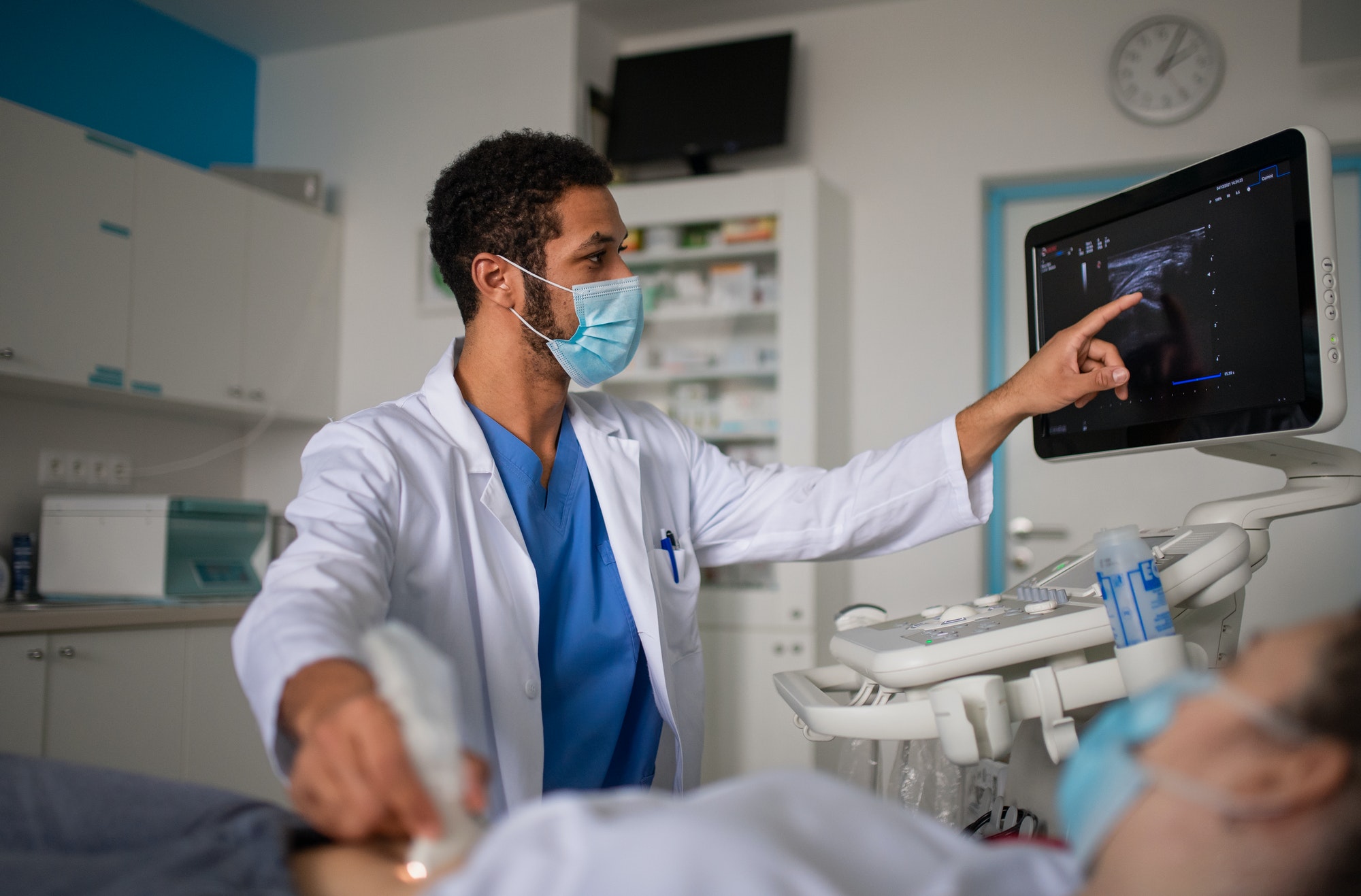
Tele-ICUs enable intensivists and other critical care professionals to leverage technology to improve access and quality of care for the critically ill. However, to realize the full benefits, hospitals must optimize their tele-ICU workflows to promote effective and timely interventions.
Here are some tips for streamlining tele-ICU operations:
- Define clear roles and responsibilities – Proactively communicate expectations for both the remote and bedside team to foster collaboration.
- Standardize hand-offs – Utilize checklists and structured communication to ensure continuity of care during shift changes.
- Select user–friendly software – Look for tele-ICU platforms with intuitive interfaces to help remote staff quickly prioritize and address needs.
- Create notification protocols – Develop standardized escalation policies detailing when and how to contact bedside clinicians about issues.
- Document thoroughly – Remote staff should comprehensively document assessments, recommendations, and interventions to inform decision-making.
- Enable two–way dialogue – Make it easy for bedside staff to request tele-ICU input through hotlines, chat features, etc.
- Conduct debriefs – Perform regular reviews of tele-ICU cases to identify process improvements.
- Assess technical needs – Ensure adequate connectivity, device access, and IT support to prevent workflow disruptions.
- Train and educate – Provide ongoing training on equipment use, communication protocols, and care pathways.
Optimizing workflows takes time but is key to realizing the full benefits of tele-ICU programs. A proactive focus on processes promotes teamwork, timely interventions, and better patient outcomes.
Tele-Hospitalists – Improving Inpatient Care Through Remote Monitoring
Over the past decade, telemedicine has begun transforming the practice of hospital medicine. Tele-hospitalists leverage technology to provide remote support and oversight for hospitalized patients. This emerging model aims to address challenges like overnight coverage gaps, lengthier hospital stays, and lack of specialty care access.
Some key advantages of tele-hospitalist programs include:
- After-hours coverage – Tele-hospitalists can monitor patients and communicate with nurses overnight when many hospitals lack on-site physician staffing. This facilitates timely interventions.
- Enhanced supervision – Junior on-site providers can consult tele-hospitalists for guidance on complex cases, improving quality of care.
- Reduced length of stay – Continuous physician oversight helps ensure patients are on target for discharge goals and transitioned home efficiently.
- Specialist eConsults – Obtaining quick remote input from specialists can improve diagnosis and treatment planning.
- Scalability – Tele-hospitalists can cover multiple facilities as demand fluctuates, providing flexible capacity.
- Cost savings – Remote staffing reduces expenses associated with on-site 24/7 hospitalist staffing.
- Risk management – Comprehensive overnight monitoring and documentation may reduce risks like falls and medication errors.
As technology expands possibilities for delivering care, tele-hospitalists are poised to take on an important role in driving better inpatient outcomes and experiences. Adoption is likely to accelerate in the years ahead.
Tele-Critical Care Consultants – Expertise Without Geographic Barriers
Critically ill patients often require complex care decisions that benefit from input by specialists in fields like pulmonology, cardiology, and nephrology. However, it can be challenging for smaller hospitals to have immediate access to this high-level expertise around the clock. Tele-critical care services are now addressing this gap.
With tele-critical care, clinicians can consult virtually with board-certified tele-intensivists who have years of ICU experience. Some applications include:
- Guide bedside teams on ventilator management, vasopressor titration, sepsis treatment, and other interventions.
- Perform comprehensive reviews of systems and data to enhance diagnosis and management.
- Advise on appropriate transfer triage when advanced therapies like CRRT or ECMO are indicated.
- Provide real-time support during emergencies and codes to optimize interventions.
- Improve standardization of care and compliance with evidence-based protocols.
- Reduce unnecessary ICU days through effective discharge planning.
- Decrease moral distress by offering reassurance and guidance in complex cases.
By tapping into specialized expertise remotely, hospitals can elevate care quality, improve outcomes, enhance clinician support, and boost patient and family satisfaction. Tele-critical care expands possibilities for team-based, patient-centered ICU practice.